If you’re stuck between “Is this a UTI or a kidney stone?” you’re not alone—because the two can overlap in annoying ways: urinary urgency, burning, lower abdominal discomfort, even blood in the urine.
Here’s the practical clinical truth: the pain pattern and “system symptoms” (fever, chills, vomiting, feeling very ill) usually tell the story fastest, and a urine test ± imaging confirms it.
Educational only. Not medical advice or a diagnosis.
What the Urinary Tract Actually Does (and What’s Involved)
Let’s clear up the basics: the urinary tract is your body’s built-in plumbing system. Its main job? Filter out waste and excess fluid, turning it into urine—and then shuttle it from your blood and out of your body.
The parts you should know:
- Kidneys: Your natural filters, working behind the scenes 24/7.
- Ureters: Tiny tubes carrying urine down from each kidney.
- Bladder: The holding tank where pee waits until you’re ready.
- Urethra: The last exit route.
Each piece plays a role, but when trouble hits (like stones or infection), where you feel it—and how—depends on which part is affected.
UTI vs Kidney Stone (quick answer)
It’s more likely a UTI if…
- Burning when you urinate plus frequent urination and lower pelvic pressure/cramping are the main features. The CDC lists these as common bladder infection (cystitis) symptoms.
- A UTI (urinary tract infection) is an infection that can occur anywhere along your urinary tract—including your urethra, bladder, ureters, or even your kidneys. UTIs are almost always caused by bacteria sneaking into your urinary system and multiplying. They’re surprisingly common: about 60% of women and 12% of men will experience at least one UTI in their lives.
- You may see blood in urine, and symptoms can feel “irritating” more than “wave-like.”
It’s more likely a kidney stone if…
- Pain is severe, often one-sided (flank/side/back), and tends to come in waves and move/radiate. Mayo Clinic describes kidney stone pain that can fluctuate and radiate, often toward the lower abdomen/groin.
- You may also have nausea/vomiting and blood in urine. NIDDK lists sharp pain (often lower back), blood in urine, nausea/vomiting among common kidney stone symptoms.
Symptom comparison
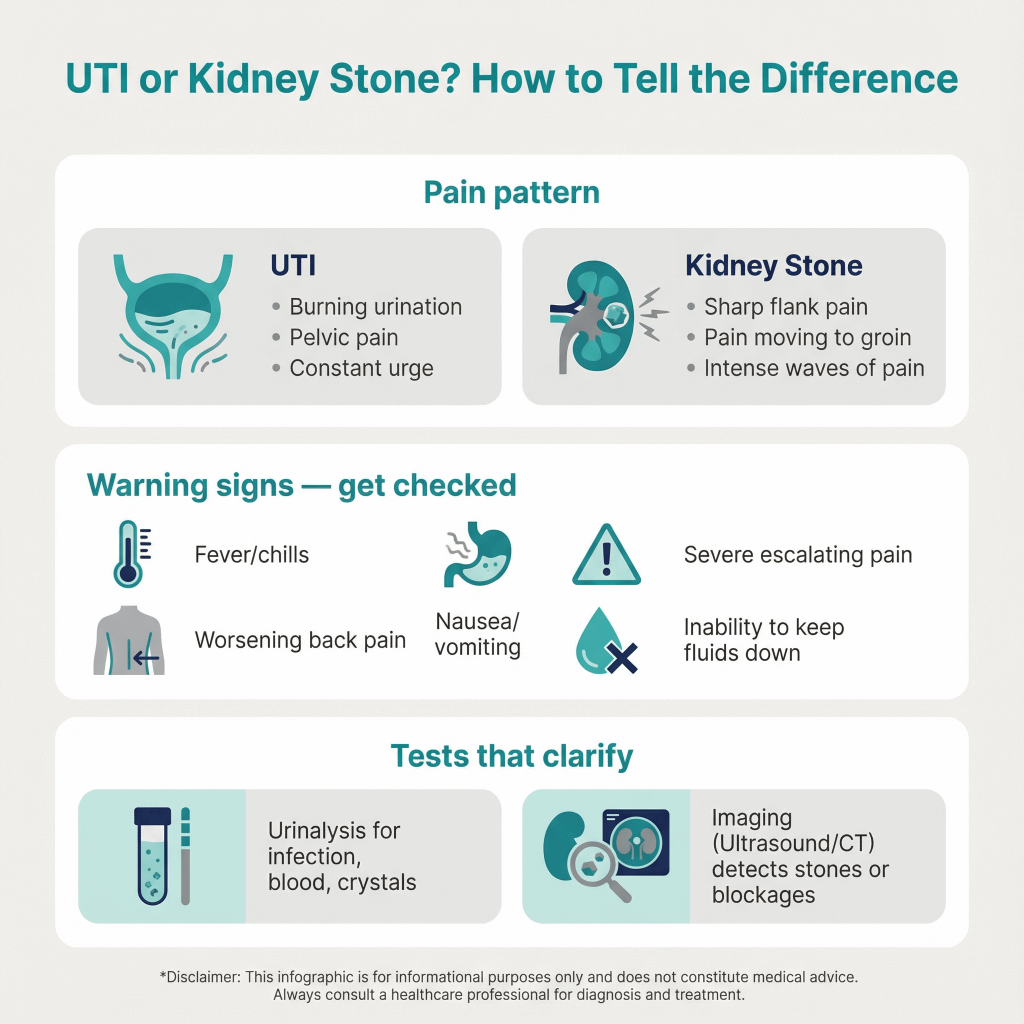
Pain location and pattern
- UTI (bladder infection): discomfort tends to stay low (lower abdomen/pelvis) with burning and urgency.
- Kidney stone: pain is often side/back (flank), may be intense, and can radiate toward the groin and worsen in waves.
Fever and chills change the priority
If you have fever + chills + back/side pain (and especially nausea/vomiting), clinicians worry more about kidney infection (pyelonephritis), which needs prompt evaluation. The CDC lists kidney infection symptoms as fever, chills, lower back/side pain, nausea/vomiting.
Blood in urine can happen with both
- CDC lists bloody urine as a possible bladder infection symptom.
- Kidney stones commonly cause blood in urine as well.
Can you have both a UTI and a kidney stone? Yes.
This is where people get confused—and it’s a legitimate overlap.
- Bacterial infections can cause struvite stones, and
- Kidney stones can increase risk for kidney infection and frequent UTIs.
So if symptoms are mixed (stone-like pain plus infection symptoms), it’s not “either/or.” It can be both—and that’s a scenario clinicians take seriously.
What tests actually tell the difference?
Urine testing
The CDC notes diagnosis may include urine tests (if needed) after symptom review and exam.
A urine culture can be used to check for bacteria/germs in urine when evaluating a suspected UTI.
Imaging (when a stone is suspected)
If a kidney stone is suspected, imaging is often used to confirm it. Mayo Clinic notes imaging tests (including CT) can show kidney stones in the urinary tract.
Cleveland Clinic summarizes that providers use imaging + blood and urine tests to diagnose kidney stones.
What are the typical treatments for kidney stones?
Kidney stone treatment really comes down to size, location, and how much misery you’re in.
- Small stones: If your stone is tiny and not causing complications, you may just need to drink lots of water, strain your urine (yes, with a filter or strainer—fun times), and let nature do its thing. Over-the-counter pain relievers can help you manage discomfort as the stone passes.
- Larger or stubborn stones: When stones get stuck, cause severe pain, or aren’t moving after a reasonable wait, doctors may talk about procedures like extracorporeal shock wave lithotripsy (yes, the fancy machine that uses sound waves to break up stones so you pee out the fragments). For bigger or more problematic stones, minimally invasive surgeries—such as ureteroscopy or, in rare cases, percutaneous nephrolithotomy—may be recommended.
- Prevention basics: Once you’ve encountered a kidney stone, you’ll want to avoid Round 2. Staying hydrated is the most consistent advice. Limiting foods high in oxalate (think spinach, beets, chocolate, nuts) can help some people, as can moderating salt and animal protein.
Treatment plans always depend on your unique situation and medical history, so your provider will help tailor the approach—with an eye on both immediate relief and keeping future stones at bay.
Who is more prone to UTIs or kidney stones?
UTI risk tends to be higher if…
The CDC notes UTIs are more common in females due to anatomy, and lists risk factors such as prior UTIs, recent sexual activity, pregnancy, menopause-related flora changes, older age, and structural issues (e.g., enlarged prostate). In fact, UTIs are surprisingly common: about 60% of women and 12% of men will experience at least one UTI in their lifetime.
Some people are more prone due to:
- A history of previous UTIs
- Increased sexual activity
- Pregnancy (which can alter urinary tract dynamics)
- Menopause, which changes the balance of protective bacteria
- Older age
- Structural or functional urinary tract issues, such as an enlarged prostate or urinary retention
Understanding these risk factors can help you recognize if you’re in a higher-risk group—and may explain why some people seem to have recurrent issues, while others rarely do.
Kidney stone risk tends to be higher if…
Kidney stones are often linked to urine chemistry and hydration status. Cleveland Clinic notes stones form when urine has too many stone-forming substances and too little liquid, and highlights dehydration as a risk factor.
Kidney stones themselves are hard mineral deposits that form in your kidneys, usually from substances like calcium, oxalate, or uric acid. They can vary greatly in size and shape—anywhere from a grain of sand to the size of a ping pong ball. When urine becomes concentrated (think: not drinking enough water or losing fluids through heavy sweating), these substances are more likely to crystallize and clump together, setting the stage for stone formation.
Other risk factors include a personal or family history of stones, diets high in salt, protein, or sugar, certain digestive diseases or surgeries, obesity, and some metabolic conditions. People who have had kidney stones before are at higher risk of developing them again.
Are there lifestyle or dietary changes that can help prevent UTIs or kidney stones?
Absolutely—prevention often starts with what you drink (and don’t drink).
UTI prevention tips include:
- Staying well-hydrated—aiming for a good amount of water each day helps flush bacteria from the urinary tract.
- Limiting bladder irritants, like caffeine, alcohol, and highly spicy foods, which can aggravate symptoms or make the bladder lining more sensitive.
- For some, urinating after sexual activity and avoiding holding urine for extended periods may also reduce risk.
Kidney stone prevention often focuses on:
- Drinking plenty of fluids—sufficient hydration dilutes the substances in urine that can crystallize and form stones.
- Watching intake of high-oxalate foods (like spinach, beet greens, nuts, and chocolate) if you’re prone to certain types of stones. The National Kidney Foundation offers helpful resources for tailored dietary tips based on stone type.
- Reducing excessive salt and animal protein can help lower risk for some stones.
Both conditions benefit from proactive hydration and thoughtful dietary choices—which can be a simple but powerful step toward preventing future problems.
How common are kidney stones?
Kidney stones are surprisingly common—Mayo Clinic estimates that about 1 in 10 people will experience a kidney stone at some point in their lives. That means millions deal with these stones over time, making it a frequent issue seen by urologists and primary care providers alike. Rates can vary based on age, sex, geography, and lifestyle, but kidney stones are not rare—so if you’ve had one (or more), you’re definitely not alone.
Warning symptoms that shouldn’t wait
If you’re trying to decide whether to “watch it” or get checked, these are the symptoms that shift the risk:
- Fever or chills with urinary symptoms
- Back/side (flank) pain plus nausea/vomiting
- Severe pain that is escalating or unmanageable
- Inability to keep fluids down (dehydration risk)
- Confusion, severe weakness, or feeling rapidly worse (especially with fever)
If infection is suspected, remember: UTIs are typically treated with antibiotics prescribed by a clinician.
What to expect if you seek care
If you’re in Houston and your symptoms fit the “warning symptoms that shouldn’t wait,” it’s reasonable to get evaluated—especially if fever/chills or severe flank pain is in the picture.
When you’re seen, your provider will review your symptoms and medical history, then order appropriate tests—usually a urine test to check for infection, and, if a kidney stone is suspected, imaging such as CT or ultrasound.
Treatment for UTIs typically involves a course of antibiotics to clear the infection. It’s important to finish all prescribed medication, even if you start feeling better within a few days. In addition, staying hydrated and avoiding caffeine, alcohol, and spicy foods may help with symptoms and reduce the risk of recurrence.
Treatment for kidney stones depends on their size and location. Small stones may pass on their own with increased fluid intake and symptom management, while larger or stuck stones sometimes need additional intervention, such as shock wave therapy or, in more significant cases, surgical removal. Preventive advice often includes drinking plenty of water and avoiding foods high in oxalates (think spinach, beet greens, chocolate) to help reduce future stone risk.
Bottom line: Don’t ignore warning signs. Prompt evaluation can get you feeling better faster and help prevent complications.
Post Oak ER states it is a freestanding ER in the Post Oak/Galleria area with board-certified physicians available 24/7.
They also state they’re located off San Felipe St. near The Galleria and Uptown Park, serving patients across Houston (including areas like Uptown, Energy Corridor, Westchase, Midtown, and the Heights).
For diagnostics, Post Oak ER describes on-site labs and imaging, including CT, X-ray, and ultrasound.
