Hearing “stage 4 kidney disease” can feel like the floor drops out from under you. The truth is: stage 4 is serious, but it is also a stage where good medical planning can make a real difference—not just for your kidneys, but for your heart, your energy, and your safety.
This guide explains what stage 4 chronic kidney disease (CKD) means, what symptoms people actually feel, what tends to cause it, and how doctors approach treatment—plus warning symptoms that shouldn’t wait.
Educational only. Not medical advice or a diagnosis.
Navigating the Emotional Side of Stage 4 CKD
Dealing with stage 4 CKD isn’t just about numbers and lab results—it’s also about handling the emotional rollercoaster that comes with it. Anxiety, sadness, or even frustration are common, and you’re not alone if you find yourself grappling with stress about what’s next.
What actually helps? For many people, talking openly with providers makes a surprising difference—especially when it comes to fears about the future or how CKD might affect everyday life. Seeking support from trusted friends, family, or even connecting with others going through CKD can lighten the emotional load.
If you’re feeling overwhelmed, don’t hesitate to ask your care team about mental health support. Many hospitals and clinics have social workers, counselors, or even local chapters of the National Kidney Foundation that offer resources designed just for patients coping with kidney disease.
A few self-care strategies people find helpful:
- Stay connected: Call a friend, join a support group, or chat with someone who “gets it.”
- Get moving (if your doctor says it’s safe): Even short walks or gentle stretching can lift your mood.
- Try mindfulness practices: Simple breathing exercises, meditation apps, or journaling can quiet the mental chatter.
- Educate yourself: Sometimes, the scariest part is not knowing. Reliable information can give you back a sense of control.
Most importantly, remember: asking for help isn’t a sign of weakness—it’s a smart part of the plan. Your kidney team wants to support all of you, not just your labs.
What does stage 4 kidney disease mean?
Stage 4 CKD means you have a severe loss of kidney function. The National Kidney Foundation defines stage 4 as an eGFR between 15 and 29 for 3 months or more (with repeat testing to confirm it isn’t a short-term kidney injury).
The American Kidney Fund also describes stage 4 CKD as eGFR 15–29, and notes it is the last stage before kidney failure, which is why planning matters here.
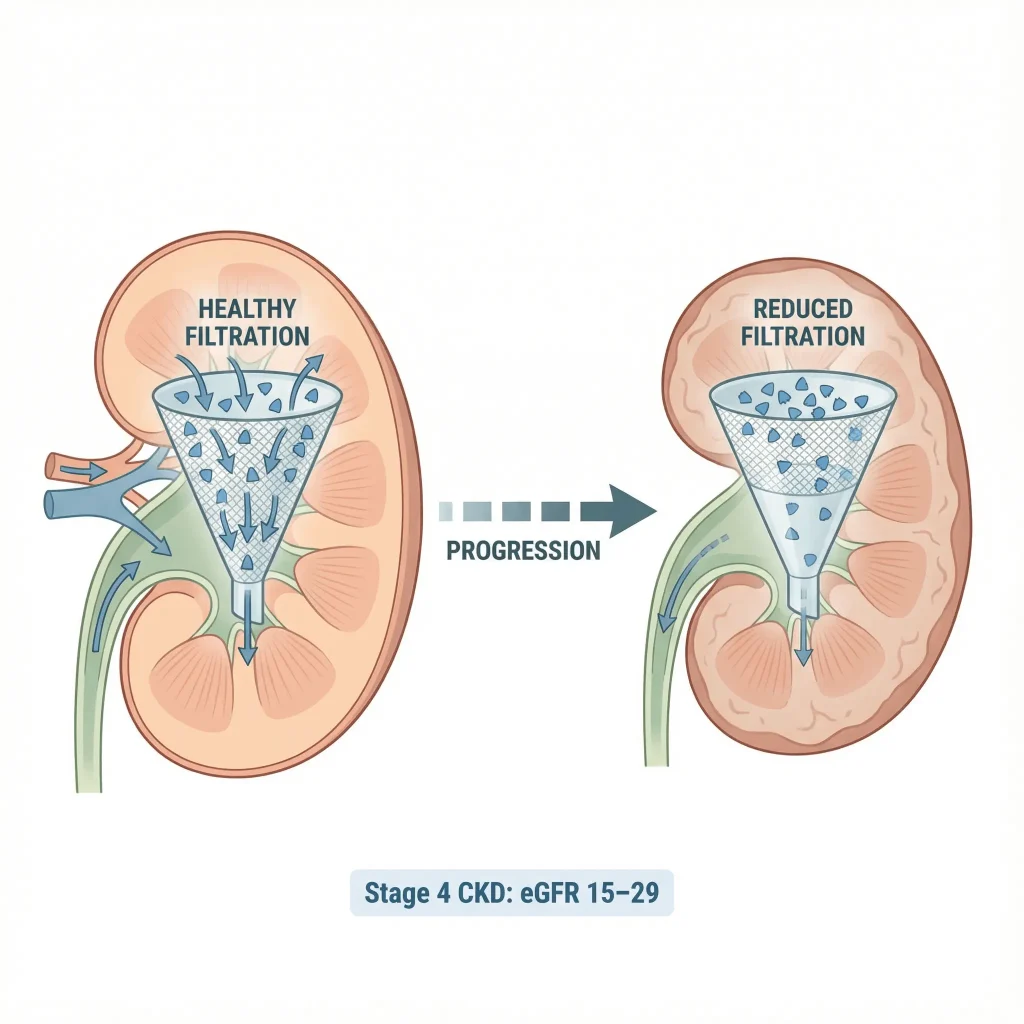
Why the numbers (eGFR 15–29) matter
At this stage, the kidney’s ability to remove waste and balance fluids/minerals is significantly reduced. That’s why people often start feeling symptoms—and why clinicians watch closely for complications.
How common is kidney disease in the U.S.?
CKD is more common than most people realize: the CDC notes more than 1 in 7 U.S. adults may have CKD, and as many as 9 in 10 don’t know they have it.
That’s one reason stage 4 is frequently discovered after years of quiet progression.
Stage 4 kidney disease symptoms
Symptoms are common in stage 4 CKD. The National Kidney Foundation lists symptoms such as:
- Urinating more or less than usual
- Itchy and/or dry skin
- Feeling tired; trouble concentrating
- Numbness or swelling in arms/legs/ankles/feet
- Achy muscles or cramping
- Shortness of breath
- Nausea and/or vomiting; loss of appetite
- Trouble sleeping
- Breath that smells like ammonia (urine-like/fishy)
these symptoms can overlap with many other conditions. What matters most is trend and whether symptoms are escalating.
What causes stage 4 chronic kidney disease?
Stage 4 CKD usually reflects long-term kidney damage. Across U.S. populations, diabetes and high blood pressure are major risk factors, and are consistently emphasized in national kidney disease education and statistics.
Other contributors can include chronic inflammation, obstruction, recurrent infections, or inherited kidney conditions—but in real-world clinical practice, diabetes and hypertension remain the most common drivers.
How do doctors figure out the cause?
To understand what’s behind an individual’s CKD, doctors may order additional tests to pinpoint the root cause and guide treatment. These may include:
- Blood pressure checks — to monitor for hypertension, a leading culprit.
- Urine tests — looking for protein, blood, or other markers of kidney injury.
- Imaging tests — such as ultrasound, CT scan, or MRI, to visualize structural changes or obstructions.
- Kidney biopsy — sometimes, a small tissue sample is needed to look for scarring or specific disease types under a microscope.
- Genetic testing — if there’s suspicion of a rare or inherited kidney disorder.
Piecing together these results helps clinicians target the right management plan and catch any underlying issues that could worsen kidney function.
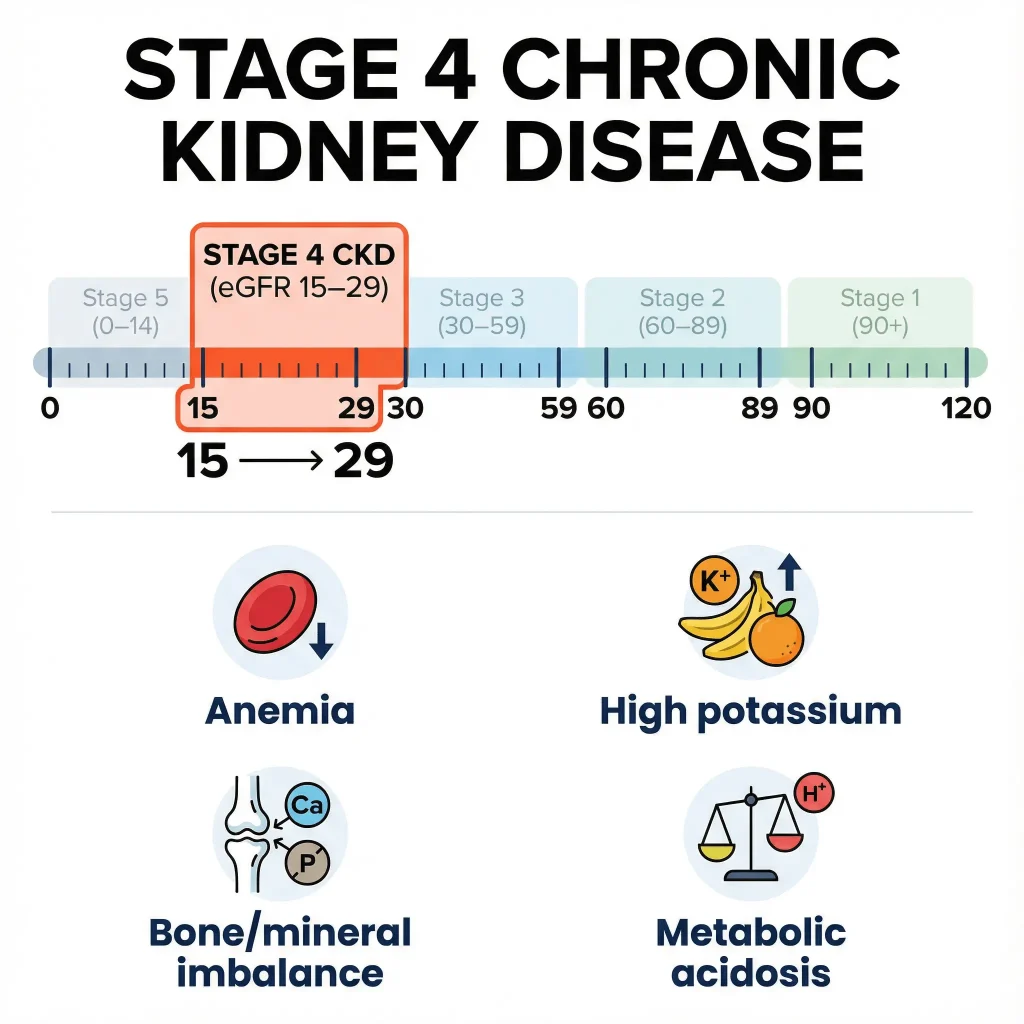
Complications in stage 4 CKD (what doctors monitor closely)
Stage 4 is also the stage where complications often become more common. NKF highlights several key complications clinicians monitor with blood tests, including:
- Anemia (low red blood cells)
- Metabolic acidosis (acid buildup)
- Mineral and bone disorder (calcium/phosphorus imbalance affecting bone and heart health)
- Hyperkalemia (high potassium)
NKF also notes stage 4 carries a very high risk for heart disease and the highest risk for kidney failure, which is why follow-up is not optional at this stage.
Is stage 4 kidney disease reversible?
In most cases, stage 4 CKD reflects chronic, established damage, so it typically isn’t “reversed” in the way an infection is cured.
However, there is still meaningful room to help:
- slow progression
- reduce complications
- and plan early for what comes next
NKF explicitly notes that even with careful treatment, kidneys may still fail—but steps taken now still help in the long run.
How long can a person live with stage 4 kidney disease—and what shapes life expectancy?
There’s no single timeline for how long someone might live with stage 4 CKD. Life expectancy can vary widely, and the numbers you’ll see online rarely tell the full story—because what matters most are details unique to you.
A few key factors play a major role:
- Age at diagnosis: Younger people often have a different outlook compared to those diagnosed at older ages.
- How well you stick to your treatment plan: Closely following recommendations, managing blood pressure, diabetes (if present), proper medications, and regular follow-up all make a difference.
- Protein in urine (albuminuria): Albumin levels (particularly if elevated) help clinicians predict risk for progression—higher numbers mean higher risk, so monitoring this with your healthcare team is critical.
- Other health conditions: The presence of heart disease, diabetes, high blood pressure, or other chronic illnesses can affect both kidney health and overall life expectancy.
Bottom line: even at stage 4, proactive care and close management can slow decline and help many people maintain quality of life for years—not just months. Every case is different, so it’s crucial to talk with your doctor about your individual risks and outlook.
The two tests that guide decisions: eGFR and urine albumin (uACR)
Even in stage 4, urine albumin (protein leakage) remains clinically important.
NKF notes that while uACR isn’t required to confirm CKD at stage 4, checking it still helps complete the picture of kidney health.
Treatment for stage 4 CKD
Stage 4 care is usually built around three goals:
- protect remaining kidney function
- reduce cardiovascular risk
- plan ahead so you’re not making urgent decisions during a crisis
Control blood pressure and diabetes
NIDDK calls controlling blood pressure the most important step for many people with CKD, and emphasizes glucose control when diabetes is present.
Managing these conditions is crucial—not just to help protect the kidneys, but also to reduce the risk of complications like heart disease. For most people, this means:
- Keeping blood pressure at the target set by your care team.
- Maintaining healthy blood sugar levels (if you have diabetes).
Regular follow-up with a nephrologist (kidney specialist) is recommended at this stage. Your kidney doctor will help coordinate your treatment plan, which often includes medicines that address both symptoms and common complications of stage 4 CKD, such as high blood pressure and diabetes. Even if you don’t have high blood pressure or diabetes, these medications may still play a role.
Medications that may slow progression
NIDDK notes that ACE inhibitors and ARBs may slow kidney disease and delay kidney failure, even in people who don’t have high blood pressure. These medications are often prescribed for their protective effect on the kidneys and, in many cases, to help manage blood pressure and support heart health.
Other medicines may be added as needed to address anemia, bone and mineral disorders, or metabolic acidosis, depending on your specific lab results and symptoms. Your care team will individualize your treatment to help keep your kidneys working as long as possible.
Nutrition changes
As CKD advances, nutrition often needs to be more intentional. NIDDK explains that choosing healthy foods and avoiding foods high in sodium, potassium, and phosphorus (when appropriate for your labs) may prevent or delay some CKD-related problems.
Why work with a dietitian?
A registered dietitian is a key part of your stage 4 CKD team. They’ll help tailor your food choices to support what your kidneys need now—focusing on the right balance of protein, sodium, potassium, and phosphorus based on your latest labs. Dietitians can translate the science into real-life meals, working with your favorite foods and cultural preferences, and adjusting guidance as your condition or medications change. In other words: they help you stay nourished, manage CKD complications, and make food less of a guessing game as needs shift over time.
Physical activity: why it matters in stage 4 CKD
Staying physically active isn’t just “nice to have”—it’s one of the few lifestyle changes that can make a clinical difference in stage 4 kidney disease.
Regular movement (think brisk walking, cycling, swimming, even gardening) can help:
- Lower blood pressure
- Improve blood sugar control
- Reduce inflammation
- Support heart health (crucial, given CKD’s link with heart disease)
- Maintain muscle strength and energy
The National Kidney Foundation and CDC both highlight the value of aiming for at least 30 minutes of moderate activity on most days. If fatigue or symptoms make even that feel daunting, talk with your care team—many find that even short bouts of gentle movement add up.
The bottom line: while exercise won’t “cure” kidney disease, it may help slow progression and reduce complications, all while boosting mood and quality of life.
Be cautious with OTC meds
NIDDK warns that NSAIDs (common pain and cold medicines that include ibuprofen/naproxen) can damage kidneys and may contribute to acute kidney injury—especially in people with kidney disease and other risk factors.
Planning ahead (dialysis/transplant decisions start here)
Stage 4 is the phase where doctors often begin structured planning for kidney failure treatment options. NKF even includes specific “planning ahead” questions such as when dialysis or transplant might be needed and how to start the process.
American Kidney Fund similarly emphasizes that stage 4 is the last stage before kidney failure and is a time to plan ahead for possible treatments.
You do not need to panic—but you do need a plan.
This is also when your nephrologist will help determine if your kidneys are nearing failure, and if so, discuss your treatment options in detail. These typically include:
- Dialysis: A treatment that cleans your blood when your kidneys can’t do the job themselves.
- Kidney transplant: Surgery that gives you a healthy kidney from a donor.
It’s worth knowing that you may be eligible to join the transplant waitlist once your eGFR drops to 20 or below, but experts recommend starting the conversation while your GFR is still between 25 and 30. Beginning the planning process early—even before you reach end-stage kidney failure—gives you extra time to learn about your choices, explore the steps involved in transplantation, and prepare for what’s ahead.
Warning symptoms that shouldn’t wait (when ER evaluation is reasonable)
Stage 4 CKD does not automatically mean “ER,” but certain symptoms can signal fluid overload, severe electrolyte issues, infection, or rapid worsening.
Consider urgent evaluation if you have:
- Shortness of breath, especially new or worsening
- Persistent vomiting or inability to keep fluids/meds down
- Rapidly worsening swelling in legs/feet/face
- Significantly reduced urination compared to your baseline
- New confusion, severe weakness, fainting, or chest pain (these can overlap with multiple emergencies and should not be observed at home)
If you’re unsure, it is generally safer to get checked than to wait for a preventable decline.
If you’re in Houston and dealing with warning symptoms that shouldn’t wait, Post Oak ER states it is located right off San Felipe St. near The Galleria and Uptown Park, and is easy to reach from areas like Uptown, the Energy Corridor, Westchase, Midtown, and the Heights.
They also state they’re open 24/7 with board-certified physicians, and provide on-site labs and imaging (including CT/X-ray/ultrasound).
Frequently Asked Questions
Is stage 4 kidney disease the same as kidney failure?
Stage 4 is not kidney failure, but it is the last stage before kidney failure (stage 5), which is why planning begins here.
What is the eGFR range for stage 4 CKD?
Stage 4 CKD is eGFR 15–29 for 3+ months.
What symptoms are common in stage 4 kidney disease?
NKF lists symptoms such as fatigue, swelling, nausea/vomiting, shortness of breath, itching, appetite loss, cramps, sleep trouble, and changes in urination.
What labs matter most in stage 4?
At minimum: eGFR trend and urine albumin (uACR). CDC notes urine albumin results 30 or above may indicate kidney disease and may be repeated to confirm.
Can I slow progression at stage 4?
Often yes. NIDDK emphasizes blood pressure control, diabetes control, monitoring kidney tests, and medication adherence as key steps to protect kidneys.