If you’ve been told “stage 2 breast cancer” — or you’re worried because you found a lump, a skin change, or a new symptom — it’s normal to feel overwhelmed. You don’t have to have everything figured out today. But you do deserve clear, practical information: what this stage means, what symptoms matter, and when symptoms cross into “don’t wait.”
This guide explains stage 2 breast cancer in plain language, the most common symptoms people notice (including signs that aren’t a lump), who may be at higher risk, and the red-flag situations where going to the ER is the safest move.
what is stage 2 breast cancer
A “stage” describes how far cancer has spread in the body. In breast cancer, stage is based on the size and location of the tumor, whether cancer is in nearby lymph nodes or other parts of the body, tumor grade, and certain biomarkers — plus whether it has spread (metastasized) to distant organs.
In general, stage 2 breast cancer means:
- The cancer is in the breast, and it may be in nearby lymph nodes (often under the arm), and
- There is no evidence it has spread to distant parts of the body (like the lungs, liver, brain, or bones).
Stage 2A vs stage 2B
Stage 2 is commonly divided into 2A and 2B. The exact substage depends on tumor size and whether nearby lymph nodes are involved. The details matter — but the big picture is the same: stage 2 is still considered an early-stage invasive breast cancer.
A key point many people don’t hear enough: symptoms alone can’t tell you the stage. Staging requires evaluation — typically imaging and biopsy — not guesswork based on how a lump feels.
Why this matters in Houston and Harris County
Breast cancer is common, and prompt evaluation matters. In Texas, the overall female breast cancer incidence rate was 121 cases per 100,000 (2017–2021), and Texas projected 21,083 new female breast cancer diagnoses in 2024.
In Harris County, the age-adjusted breast cancer incidence rate was 117.1 cases per 100,000 females (2017–2021).
These numbers aren’t here to scare you. They’re here to say: you’re not alone, and getting checked is a normal, appropriate next step.
Common symptoms and warning signs
Different people notice different changes. Some people feel a lump. Others see a skin or nipple change first. And some people have no symptoms and find cancer through screening.
If you’re searching what are signs of breast cancer or even typing what breast cancer symptoms because something feels off, start with the symptom list below — then get a clinician involved if the change is new or persistent.
Common warning signs include:
- New lump in the breast or underarm (armpit)
- Thickening or swelling of part of the breast
- Irritation or dimpling of breast skin (sometimes “orange peel” texture)
- Redness or flaky skin in the nipple area or the breast
- Pulling in of the nipple (nipple inversion) or new nipple pain
- Nipple discharge other than breast milk (including blood)
- A visible change in breast size or shape that doesn’t go away
What does a breast cancer lump feel like?
Many people expect a cancer lump to be painful, but that’s not always true. A lump can be painless, firm, or irregular — but breast cancers can also be soft, round, tender, or even painful.
The most useful rule is simpler: any new lump that persists should be evaluated.
Can you have breast cancer without a lump?
Yes. Some breast cancers show up first as skin changes, nipple changes, swelling, or underarm lymph node swelling — not a distinct lump.
Is breast pain a sign of breast cancer?
Breast pain is common and often caused by non-cancer issues (hormonal changes, inflammation, cysts). But persistent, localized pain — especially when paired with other changes (skin dimpling, nipple discharge, swelling, or a new lump) — deserves prompt medical evaluation.
Who is more at risk?
Having a risk factor doesn’t mean you will get breast cancer — and many people diagnosed have no obvious risk factors. But risk factors help decide how closely someone should be monitored and how quickly to evaluate a new symptom.
Risk factors you can’t change:
- Being a woman and getting older (most breast cancers are found in women age 50+)
- Family history of breast cancer
- Inherited gene changes (such as BRCA mutations)
- Personal history of breast cancer or certain breast conditions
Risk factors that may be modifiable:
- Alcohol use
- Obesity/overweight (especially after menopause)
- Low physical activity
If you’re reading this and blaming yourself: please don’t. Risk is complicated, and cancer is never a moral failing.
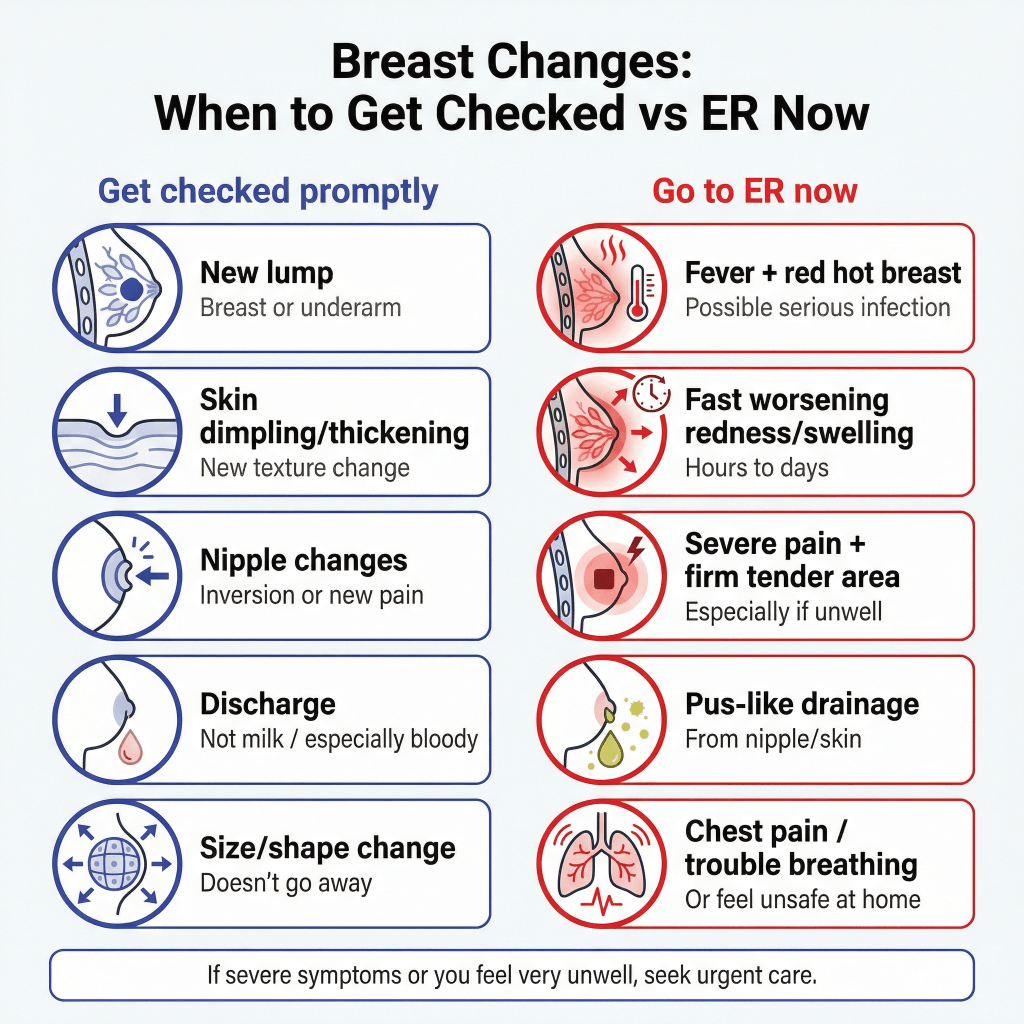
Go to the ER now (urgent red flags)
Most breast concerns should be evaluated quickly — but not all are emergencies. The ER is the right place when symptoms suggest a serious infection, rapid progression, or you feel systemically ill.
Go to the ER now if you have:
- Fever and chills with a red, hot, swollen, painful breast
- Rapidly worsening redness, swelling, or warmth over hours to a couple of days
- Severe breast pain with a firm, very tender area (especially if you feel unwell)
- Pus-like drainage from the nipple or skin
- You feel faint, confused, severely weak, or dehydrated
- Trouble breathing or chest pain, or anything that makes you feel unsafe at home
Why this matters: breast infections (mastitis) can cause swelling, redness, warmth, pain, and — if infection is present — fever and chills.
Another condition that can look similar is inflammatory breast cancer, which can cause the breast to become swollen, red, and tender often in a matter of days or weeks — and it often does not cause a breast lump.
You cannot self-diagnose the cause from appearance alone — rapid or severe symptoms should be evaluated urgently.
What ER clinicians may do next
If you come to the ER with urgent breast symptoms, clinicians may:
- Check vital signs and assess how sick you feel overall
- Perform a focused breast and lymph node exam
- Order labs if infection is suspected
- Consider imaging when appropriate (often ultrasound for certain urgent questions)
- Treat pain, fever, dehydration, and nausea as needed
- Start treatment for suspected infection when appropriate and arrange safe follow-up
- Direct you to urgent outpatient breast imaging or specialist follow-up for definitive evaluation (diagnostic mammogram/ultrasound and, if needed, biopsy)
Important boundary: the ER can identify and treat emergencies and help you get onto the right diagnostic pathway — but final staging and treatment planning usually happen through imaging, biopsy, and oncology teams outside the ER.
What you can do today
Whether your next step is the ER or an outpatient visit, these practical steps help:
- Write down what changed and when it started
- If there are visible skin changes, take a clear photo each day for comparison
- Note associated symptoms: fever, discharge, pain level, underarm swelling, fatigue
- Bring key history: family history, prior breast imaging, prior biopsies, pregnancy/breastfeeding status, and medications
- If symptoms are not emergent, schedule diagnostic breast imaging (not just screening) through your doctor or a breast center
Need Urgent Evaluation for Breast Symptoms?
A new breast change can be frightening — especially when symptoms are getting worse fast. If you have fever, severe pain, rapid swelling, spreading redness, pus-like drainage, chest pain, or shortness of breath, don’t delay care.
Post Oak ER is here 24/7 to evaluate emergency breast symptoms, rule out serious complications, and help you take the safest next step.
Come in now if your symptoms feel urgent, severe, or are worsening quickly.
Frequently Asked Questions
Is stage 2 breast cancer curable?
Many stage 2 breast cancers are treated with curative intent, but no one can promise a cure for an individual person. Prognosis depends on factors like tumor biology (hormone receptors, HER2), grade, lymph node involvement, and overall health. Population survival statistics can help with context, but they don’t predict a single person’s outcome.
Can stage 2 breast cancer spread to bones?
Stage 2 means there is no evidence of distant spread at diagnosis. However, breast cancer can spread later in some cases, which is why timely treatment and follow-up matter. If you develop new, severe, unexplained symptoms — especially persistent pain that’s getting worse or major shortness of breath — seek urgent evaluation.
What are the early signs of breast cancer?
Early signs can include a new breast or underarm lump, thickening, dimpling, nipple inversion, nipple discharge, or a change in breast size/shape. Some people have no symptoms at all, which is why screening can matter.
What are the 5 warning signs of breast cancer?
A simple “top five” to remember:
New breast or underarm lump
Thickening/swelling of part of the breast
Skin dimpling or irritation
Nipple changes (pulling in, pain, scaling)
Nipple discharge that isn’t breast milk (including blood)
What does a breast cancer lump feel like, and do breast cancer lumps hurt?
People ask this a lot — and the truth is: it varies. A lump can be painless, firm, and irregular — but it can also be tender or painful. Pain doesn’t rule cancer in or out. If you’re searching do breast cancer lumps hurt, the safest takeaway is: new + persistent = get it checked.
People also ask what does a breast cancer lump look like — often it isn’t visible at all, and the first visual sign can be skin pulling/dimpling or swelling rather than a “bump.”
Can you have breast cancer without a lump?
Yes. Some cancers present with nipple discharge, nipple inversion, skin dimpling, redness or scaling, swelling, or an underarm lump rather than a distinct breast lump.

