Key Takeaways
- Your occipital lobe sits at the back of your brain and is a major hub for visual processing—so a stroke there can show up as a vision problem first.
- Stroke-related vision symptoms are often sudden: trouble seeing in one or both eyes, missing part of your visual field, new double vision, or sudden balance trouble.
- An occipital-lobe stroke can cause visual field loss even without other obvious stroke symptoms—which is one reason people delay.
- If stroke is suspected: Call 911 for severe symptoms / suspected stroke.
What does the occipital lobe do, and why does stroke there affect vision?
If you only remember one thing about the occipital lobe, it’s this: it helps your brain make sense of what your eyes are seeing.
Cleveland Clinic describes the occipital lobe (at the back of the brain) as home to your brain’s visual processing abilities—and it helps connect what you see with other brain functions.
That matters because a stroke is basically a “blood flow emergency.” When blood flow is blocked (ischemic stroke) or a vessel bleeds (hemorrhagic stroke), the part of the brain downstream can stop working normally. The CDC explains stroke as a brain event where blood flow problems lead to brain injury, and one of the classic warning signs is sudden trouble seeing in one or both eyes.
So if the stroke affects the occipital lobe—your “vision processing zone”—you can get symptoms like:
- sudden blurry vision,
- sudden loss of vision in part of the visual field,
- trouble reading or recognizing what you’re seeing,
- or “something is missing” on one side of what you see.
And here’s the tricky part: you might not have chest pain, you might not have a headache, and you might not have obvious arm weakness. You might just have a vision problem that feels “eye-related.”
That’s exactly how people lose time.
What is an occipital lobe stroke?
An occipital lobe stroke is simply a stroke that injures the occipital lobe. Stroke itself comes in two main pathways:
- Ischemic stroke (blocked blood flow), and
- Hemorrhagic stroke (bleeding).
Whether the cause is blockage or bleeding, the result is that brain tissue doesn’t get what it needs—oxygen and nutrients—and neurologic symptoms show up quickly. The CDC’s warning-sign list includes sudden trouble seeing as a key symptom because visual pathways are part of the brain’s “high-demand” circuitry.
Why occipital strokes feel “different”
Most people think “stroke” means:
- face droop,
- arm weakness,
- slurred speech.
Those are absolutely real and common.
But occipital strokes can show up as vision-first problems—which makes people:
- wait for it to pass,
- call it “fatigue,”
- blame a screen,
- or assume it’s a normal eye issue.
Sometimes it is an eye issue. But the cost of guessing wrong is too high.
Vision symptoms that can signal an occipital-lobe stroke

Sudden trouble seeing in one or both eyes
This is not a “maybe.” Both the CDC and American Stroke Association list sudden trouble seeing in one or both eyes as a stroke warning sign.
People describe it as:
- “everything suddenly went blurry,”
- “I can’t see out of one side,”
- “my vision is dim,”
- “it feels like a curtain,”
- “I can’t focus even though my glasses are fine.”
The key word is sudden—especially if it’s new for you.
Visual field loss
One of the most classic stroke-related vision issues is visual field loss, meaning part of what you see is missing—even though the eyes themselves may be okay.
This can look like:
- bumping into door frames or people on one side,
- reading only the left half of a sentence,
- missing food on one side of a plate,
- feeling “clumsy” in crowded places.
And here’s a detail that really matters for this specific blog: an NHS hospital patient leaflet notes that strokes affecting the very back of the brain (the occipital lobe) may cause visual field loss without any other problems.
So if someone says, “No weakness, no speech issue—just vision,” that does not rule out stroke.
Double vision (diplopia)
Sudden double vision can be alarming—and it should be taken seriously.
Mayo Clinic’s TIA (mini-stroke) symptom list includes blindness in one or both eyes or double vision, along with dizziness/balance problems.
That tells you something important: double vision can be part of a brain blood-flow event, not just an eye problem.
Cleveland Clinic also emphasizes that you should get sudden double vision checked promptly and that sudden changes in vision can signal something serious.
Practical rule: new, sudden double vision—especially with dizziness, imbalance, weakness, speech trouble, or a “not right” feeling—should be treated as urgent.
“My eyes are fine, but my brain can’t process what I’m seeing”
Some post-stroke vision issues aren’t just blur or missing vision. They’re processing issues:
- trouble recognizing objects,
- trouble reading,
- difficulty judging distance,
- difficulty processing motion.
Cleveland Clinic notes the occipital lobe links sight with other senses/brain abilities—so injury can affect how vision is interpreted, not just whether light reaches the eye.
When to call 911 for vision symptoms
The CDC says to call 9-1-1 right away if you or someone else has stroke warning signs— including sudden trouble seeing.
The American Stroke Association says to call 911 immediately if you observe even one stroke symptom and highlights the urgency: on average, 1.9 million brain cells die every minute a stroke goes untreated.
The “sudden + new + neurologic” rule
Treat it as an emergency if the vision change is:
- sudden, and
- new, and
- comes with any neurologic sign (balance trouble, confusion, weakness, speech trouble), or
- is severe (sudden major vision loss, new double vision, “half my vision is gone”).
Call 911 for severe symptoms / suspected stroke.
Don’t drive yourself if stroke is suspected
If stroke is on the table, the safest move is EMS. Stroke is time-sensitive and early activation matters.
(And practically—if your vision is compromised, driving is dangerous.)
If it got better: could it be a TIA (mini-stroke)?
Yes. And this is one of the biggest traps.
A TIA can cause stroke-like symptoms that resolve, sometimes quickly. Mayo Clinic notes TIA symptoms happen suddenly and can include blindness in one or both eyes or double vision, and it says if you think you’re having or have had a TIA, get medical attention right away.
NINDS also emphasizes that TIA is a serious warning event and should be treated urgently.
So if someone says:
- “My vision went weird for 10 minutes and then it cleared,”
- “I had double vision and dizziness, but now I’m fine,”
- “I couldn’t see on one side for a bit and then it resolved,”
…that is not a “we’ll watch it for a week” situation. It’s a “we need an urgent evaluation” situation, because the next event may not resolve.
What else can cause sudden vision changes?
Not every vision symptom is stroke. But you don’t want to bet your brain (or your eyesight) on guessing.
Two key points help keep this safe:
- Sudden vision loss is a medical emergency even when it’s not stroke. Cleveland Clinic says sudden vision loss (minutes to a few days) is a medical emergency and may require imaging or blood tests to find the cause.
- Some urgent eye conditions can permanently affect vision if delayed. Mayo Clinic calls retinal detachment an emergency situation.
A few serious non-stroke causes
- Retinal detachment (flashes/floaters/curtain-like loss can occur; it’s an emergency).
- Acute angle-closure glaucoma, retinal artery occlusion, giant cell arteritis, optic neuritis (AAFP lists these as common and dangerous causes of sudden vision loss).
You don’t need to memorize this list. The point is: sudden vision loss deserves urgent evaluation, whether the cause is in the eye or the brain.
What to do right now
If it’s happening now
- Call 911 if stroke is suspected—especially if vision symptoms are sudden and new, or paired with weakness, speech trouble, confusion, or balance problems.
- Note the time symptoms started (or last known well). Stroke teams treat time as critical information.
- Keep the person safe (vision changes increase fall risk).
- Don’t delay by trying to “test” the person at home. If it looks like stroke, treat it like stroke.
If it happened earlier and improved
Treat it like a possible TIA:
- Same-day urgent evaluation matters.
- Do not dismiss it because it passed.
What to expect in the ER for sudden vision changes
Here’s what typically happens:
What clinicians focus on first
- Timing: when did it start, when was the person last normal?
- A focused neurologic exam (including balance/coordination and vision checks)
- Vitals and quick checks for common “mimics” (like blood sugar issues)
- Deciding whether the pattern looks more like an eye emergency, a brain emergency, or both.
Common evaluation categories
Depending on the story, clinicians may consider:
- brain imaging to evaluate for stroke/bleeding,
- lab work,
- heart rhythm evaluation (because some strokes relate to rhythm issues),
- and/or urgent eye evaluation if eye pathology is suspected.
Again: the goal is to explain why urgent evaluation is warranted for sudden vision symptoms.
Recovery and outlook: vision problems after stroke
This is the part families ask about quietly: “Will their vision come back?”
The honest answer: it depends, but improvement is possible.
- The Stroke Foundation notes vision changes affect about one third of stroke survivors, that vision may improve, but full recovery is less common, and recovery tends to happen most in the first few months.
- UK Stroke Association materials also emphasize that vision problems are common after stroke and include visual field loss and processing issues.
Is vision loss from stroke permanent?
Sometimes. Sometimes not. It varies based on:
- where the stroke occurred,
- how much tissue was affected,
- overall brain health,
- and what rehabilitation/support is used.
The most responsible thing to tell a patient is: don’t assume permanence early—and don’t assume full recovery either. Get evaluated, then follow the recovery plan you’re given.
How long do vision problems last after a stroke?
Many people see the most change early, especially in the first months, but some continue improving later.
And even when vision deficits persist, people can often improve function through strategies, therapy, and adaptations.
Does double vision after a stroke go away?
It can—depending on the cause (eye movement control vs visual processing) and the rehab plan. The key is: don’t self-manage sudden double vision. Sudden changes should be evaluated urgently because they can signal a serious neurologic or eye event.
Prevention
This article is about symptom recognition, but prevention still matters.
Stroke risk reduction usually focuses on managing major drivers like:
- blood pressure,
- diabetes,
- cholesterol/atherosclerosis,
- smoking,
- and rhythm issues (like AFib) when present.
You don’t need to perfect everything overnight. The practical goal is: lower risk and recognize emergencies early.
If you or someone around you has sudden vision loss, missing part of the visual field, new double vision, or vision changes with weakness, confusion, balance trouble, or speech changes, call 911 immediately. Post Oak ER is open 24/7 for emergency care when urgent evaluation is needed.
Frequently Asked Questions
Can a stroke affect vision?
Yes. Both the CDC and American Stroke Association list u003cstrongu003esudden trouble seeing in one or both eyesu003c/strongu003e as a stroke warning sign.
Is blurry vision a sign of a stroke?
It can be—especially when it is u003cstrongu003esudden, new, and severeu003c/strongu003e, or comes with other neurologic symptoms (balance trouble, weakness, speech trouble).
Is double vision a sign of a stroke?
It can be. Mayo Clinic includes u003cstrongu003edouble visionu003c/strongu003e among symptoms that can occur with TIA (mini-stroke). Sudden double vision should be evaluated urgently.
What vision symptoms should make me call 911 immediately?
Sudden vision loss, missing half of your visual field, sudden new double vision, or sudden trouble seeing—especially with balance trouble, confusion, weakness, or speech changes. u003cstrongu003eCall 911 for severe symptoms / suspected stroke.u003c/strongu003e
If vision symptoms come and go, could it still be a TIA (mini-stroke)?
Yes. TIAs can cause symptoms that resolve, including vision symptoms, and still require urgent medical attention.
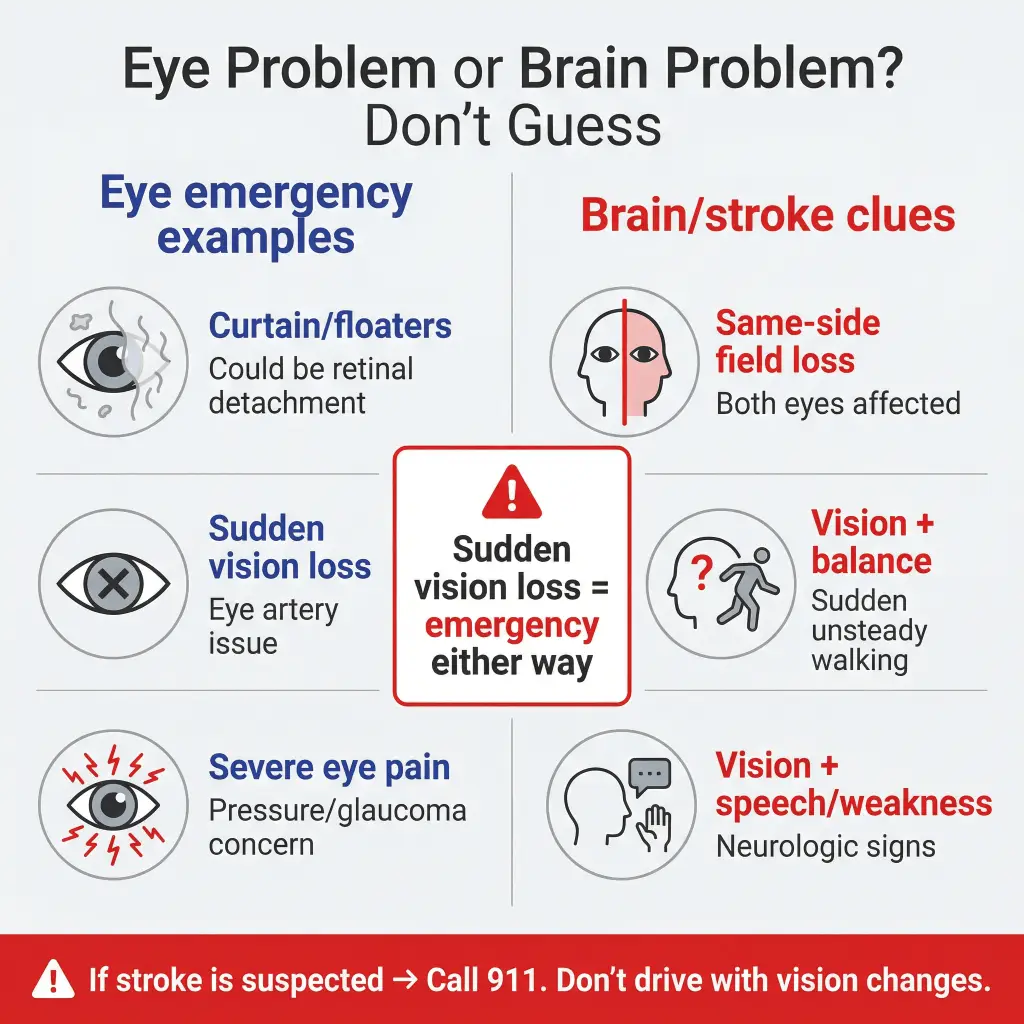
What’s the difference between an eye problem and an occipital-lobe (brain) vision problem?
Eye problems affect the eye itself; occipital-lobe problems affect how the brain processes visual information. But in real life, u003cstrongu003esudden vision loss is an emergency either wayu003c/strongu003e, and you shouldn’t try to sort it out at home.
Is vision loss from stroke permanent?
Sometimes, but vision can improve—often most in the first few months—though full recovery is less common.
How long do vision problems last after a stroke?
It varies, but reputable stroke resources note that improvement often happens most in the first few months.