Key Takeaways
- Left arm pain by itself is not the “classic” stroke symptom. Stroke more often causes sudden weakness or numbness in the face/arm/leg—especially on one side.
- Left arm pain can be an emergency, but it’s more commonly discussed as a heart attack warning sign—especially when paired with chest discomfort or shortness of breath.
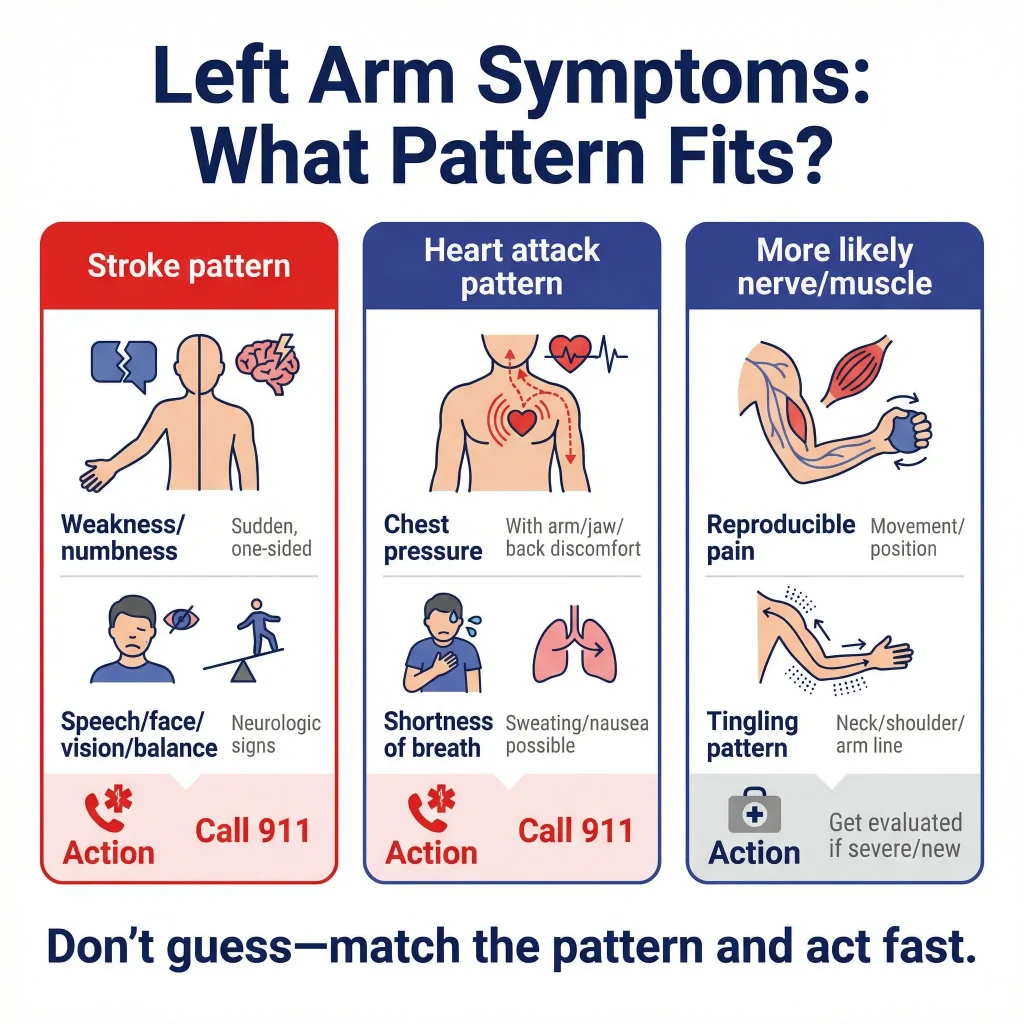
- The safest way to decide isn’t to guess the diagnosis. It’s to recognize the pattern:
- Sudden neurologic changes (face/arm weakness, speech trouble, vision/balance changes) → treat as stroke.
- Chest discomfort + arm pain (or arm/jaw/back discomfort with shortness of breath, sweating, nausea) → treat as heart attack.
- If stroke is suspected: Call 911 for severe symptoms / suspected stroke.
Can left arm pain be a sign of stroke?
Yes—but it’s not the most typical presentation.
If you ask ER doctors what “stroke in the arm” looks like, most of us won’t say “pain” first. We’ll say sudden weakness or sudden numbness—especially on one side. The CDC lists sudden numbness or weakness in the face, arm, or leg (especially one side) as a key stroke warning sign.
Pain vs weakness/numbness
- Stroke: more often weakness/numbness, sudden, one-sided.
- Heart attack: often chest discomfort and may include discomfort in one or both arms, plus other symptoms.
- Nerves/muscles/joints: can cause arm pain, tingling, numbness—usually linked to position, movement, or a clear musculoskeletal trigger. (A pinched nerve commonly causes numbness, tingling, and pain.)
The key is not the label. It’s the pattern and urgency.
What stroke arm symptoms usually look like
Sudden arm weakness
This is classic:
- One arm drifts down when trying to hold both arms up.
- A hand suddenly can’t grip like normal.
- The arm feels heavy, clumsy, or “not connected.”
The American Stroke Association’s FAST guidance includes Arm Weakness and Speech Difficulty as major indicators, and it says: call 911 immediately.
Is numbness a sign of stroke?
It can be. The CDC includes sudden numbness (especially one-sided) as a stroke warning sign.
Mayo Clinic also lists paralysis or numbness of the face, arm, or leg on one side of the body as a stroke symptom and emphasizes urgency even if symptoms come and go.
Is tingling a sign of stroke?
Tingling can show up in neurologic events, but the safest way to interpret tingling is this:
- If it’s sudden, new, one-sided, and especially paired with weakness, face changes, speech trouble, vision trouble, or imbalance → treat it like possible stroke.
- If it’s tied to position or a known nerve pattern (neck/shoulder posture, radiating pain, reproducible with movement), a pinched nerve is one possible explanation—but that’s not something you should “confirm” at home if the onset is sudden or the symptoms are severe.
What does stroke numbness feel like?
People describe it as:
- “My arm feels dead or asleep, but it’s not getting better.”
- “It’s like my arm isn’t mine.”
- “I can’t tell where my hand is unless I’m looking.”
What makes it more stroke-like is sudden onset, one-sided, and especially if it comes with any FAST symptom (face droop, arm weakness, speech change).
The “arm symptom + brain symptom” combo
Left arm pain is messy. Left arm weakness/numbness is cleaner. But what really sharpens concern is the combination:
- arm weakness/numbness plus slurred speech or trouble speaking,
- arm symptoms plus facial droop,
- arm symptoms plus sudden vision changes,
- arm symptoms plus sudden balance trouble.
Those are all on the CDC’s stroke sign list or the ASA stroke symptom guidance.
When left arm pain points away from stroke (but may still be urgent)
When it looks more like a heart problem
This is the part people don’t like to hear, but it’s important:
Left arm pain is more commonly taught as a heart attack warning sign than a stroke warning sign. The American Heart Association lists heart attack warning signs that include chest discomfort, discomfort in other upper body areas (including the arm), and shortness of breath.
NHLBI describes heart attack symptoms including chest pain/heaviness/discomfort, pain or discomfort in one or both arms (and other areas like jaw/neck/back), shortness of breath, sweating, nausea/vomiting, dizziness, and rapid/irregular heartbeat.
If left arm pain shows up with:
- chest pressure/tightness,
- shortness of breath,
- sweating,
- nausea/vomiting,
- pain spreading to jaw/neck/back…
…treat it as an emergency and call 911.
When it looks more musculoskeletal or nerve-related
Arm pain can also be:
- shoulder strain,
- tendon inflammation,
- arthritis,
- “slept wrong,”
- a pinched nerve.
A pinched nerve commonly causes numbness, tingling, and pain.
But here’s the ER caveat: a benign cause is usually something you can reproduce (movement/position) and it usually doesn’t come with sudden neurologic deficits. If you’re seeing a sudden, one-sided neurologic change, you don’t “test it at home.” You escalate.
When to call 911

If you suspect stroke
Use this as the clean rule:
If the arm symptom is sudden and paired with any of these:
- face droop,
- arm weakness,
- speech difficulty,
- sudden vision trouble,
- sudden trouble walking/balance,
- sudden severe headache…
…treat it like stroke and call 911 right away.
Call 911 for severe symptoms / suspected stroke.
If you suspect heart attack
If left arm pain shows up with chest discomfort or other classic heart attack warning signs, treat it as an emergency.
(If you’re not sure whether it’s stroke or heart attack, that’s exactly why EMS exists. You don’t have to be right—you have to be fast.)
If it got better: could it be a TIA (mini-stroke)?
Yes.
This is a common trap: “It passed, so it’s fine.”
NINDS explains that a TIA is a stroke that lasts only a few minutes; symptoms usually go away within an hour (sometimes up to 24 hours), and they are similar to stroke symptoms.
Mayo Clinic is also explicit: if you notice stroke symptoms—even if they come and go or disappear—seek emergency medical attention or call 911.
So if you had:
- sudden arm weakness/numbness that resolved,
- sudden slurred speech that resolved,
- sudden vision changes that resolved…
…don’t “wait for it to happen again.” Treat it as urgent.
What to do right now
If symptoms are happening now
- Call 911 if you suspect stroke or heart attack.
- Note the time symptoms started (or “last known well”). The ASA specifically instructs noting when symptoms first appear.
- Keep the person safe and still if they’re weak, dizzy, or confused.
- Don’t waste time trying to “prove” it’s one thing or another. If it’s sudden and concerning, treat it as an emergency.
If symptoms happened earlier and improved
Treat it like a possible TIA or warning event:
- Get urgent medical evaluation the same day.
- Don’t assume improvement equals safety.
What to expect in the ER (conservative, real-world)
I’ll keep this general and compliant—no promises about specific tests at any specific facility.
If clinicians suspect stroke
Expect a focus on:
- timing (when did it start, last-known-well),
- a neurologic exam (strength/speech/face/vision/balance),
- and an evaluation to determine whether this is blockage vs bleeding and what needs to happen next.
If clinicians suspect a cardiac cause
Expect rapid assessment aimed at ruling out heart attack or dangerous rhythm problems—often with an ECG and other testing based on clinical judgment. (NHLBI describes how symptoms can vary and include arm discomfort and shortness of breath.)
Prevention basics
This post is about emergency recognition, but prevention matters—because stroke and heart attack share a lot of risk drivers.
At a high level, risk reduction often means working with your clinician on:
- blood pressure control,
- diabetes control,
- cholesterol/atherosclerosis risk,
- smoking cessation,
- and evaluating rhythm issues (like AFib) when present.
If left arm symptoms are sudden, come with face droop, speech trouble, vision or balance changes, or happen with chest discomfort, shortness of breath, sweating, or nausea, call 911 immediately. Post Oak ER is open 24/7 for emergency care when urgent evaluation is needed.
Frequently Asked Questions
Can left arm pain be a sign of stroke?
It can, but stroke more commonly causes sudden weakness or numbness, especially on one side.
Is arm weakness more concerning than arm pain for stroke?
Yes. Sudden arm weakness is a classic stroke sign (FAST).
Is numbness a sign of stroke?
Yes—sudden numbness, especially on one side, is a key warning sign.
Is tingling a sign of stroke?
It can be, especially if it’s sudden, one-sided, and paired with other neurologic symptoms. Stroke symptom lists emphasize sudden one-sided sensory change and other neurologic deficits.
What does stroke numbness feel like compared to a pinched nerve?
Stroke numbness is often sudden, one-sided, and may come with weakness/speech/vision/balance changes. Pinched nerves commonly cause numbness/tingling/pain and may be linked to position or nerve distribution.
What other stroke symptoms often occur with arm symptoms?
Face droop, speech trouble, vision changes, balance trouble, severe sudden headache.
When should I call 911 for left arm symptoms?
Call 911 if arm symptoms are sudden and paired with any stroke warning sign, or if they occur with chest discomfort or other heart attack warning signs.
Could it be a TIA if symptoms went away?
Yes. TIA symptoms can resolve quickly and still require urgent evaluation.
Can right arm pain be a stroke?
It can be part of an emergency pattern too. Stroke symptoms can affect either side depending on which part of the brain is involved. The key is sudden neurologic change (weakness/numbness/speech/vision/balance).

