A kidney stone is a hard deposit that can form when certain minerals and salts concentrate in the urine. When a stone moves into the ureter (the narrow tube that carries urine), it can trigger sudden, intense pain and urinary symptoms.
Your kidneys are fist-sized organs, typically one on each side of your spine, tucked behind the stomach and below the ribs. Their day job? Cleaning waste from your blood and managing the delicate balance of fluids and minerals like sodium, potassium, and calcium. The kidneys, together with the ureters and bladder, make up your urinary tract—a sort of internal plumbing system that produces urine, moves it down the ureters, and stores it in the bladder until you’re ready to go.
Kidney stones form inside the kidney, but the drama often starts when one of these stones tries to leave its home turf. As urine flows out of the kidney and into the ureter, a stone can get stuck in this narrow tube. This not only blocks the flow of urine but can also cause waves of severe pain, commonly known as renal colic, and a range of urinary symptoms.
If you’re searching because you’re uncomfortable right now, here’s the core clinical takeaway: the “pattern” of pain and the presence of fever, vomiting, or trouble urinating help determine how urgent the situation is—then urine testing and imaging help confirm what’s going on.
Educational only. Not a diagnosis or personal medical advice.
what do kidney stone symptoms feel like?
NIDDK lists kidney stone symptoms that commonly include:
- sharp pains in the back, side, lower abdomen, or groin
- blood in urine (pink/red/brown)
- constant need to urinate, pain while urinating
- inability to urinate or only urinating a small amount
- cloudy or bad-smelling urine
But the full range of symptoms can be broader. Other signs you might notice include:
- a feeling of intense, sudden need to urinate
- urinating more frequently than usual
- burning sensation during urination
- urine that appears dark or red—sometimes blood is present in amounts too small to see
- nausea and vomiting (sometimes accompanying the pain)
- for men, pain that radiates to the tip of the penis
NIDDK also notes the pain may come and go in waves, and you may have nausea and vomiting; fever and chills can also occur.
Cleveland Clinic similarly describes kidney stone pain that can radiate and get worse in waves.
Kidney stone vs UTI — how to tell the difference
These can overlap, but the story often differs:
More consistent with a kidney stone
- Pain that’s one-sided (flank/back/side), often severe, and waxes and wanes in waves
- Nausea/vomiting accompanying the pain
- Blood in the urine
More consistent with a bladder UTI
- Burning and urinary urgency/frequency as the main feature (often without severe wave-like flank pain)
When the combination is more concerning
If you have urinary symptoms plus fever/chills (or you feel suddenly very sick), clinicians worry more about infection complications and want evaluation sooner. NIDDK lists fever and chills among possible kidney stone symptoms.
What causes kidney stones?
NIDDK explains kidney stones can be caused by high levels of calcium, oxalate, and phosphorus in urine.
Some people are simply more “stone-prone,” and certain foods can increase risk in those individuals.
But there’s more to the story—understanding why you get stones is key to preventing them from coming back. Your healthcare provider may ask about your personal and family medical history, such as:
- Have you had more than one stone before?
- Does anyone in your family have a history of kidney stones?
- Do you have medical conditions like frequent diarrhea, gout, or diabetes that might increase your risk?
Your diet also plays a role. Eating foods high in salt, certain proteins, or oxalate (think spinach, nuts, chocolate) can make some people more likely to form stones—especially if you’re not drinking enough fluids. On the flip side, some foods and habits help protect against stone formation.
By reviewing your medical, family, and dietary history, your provider can help pinpoint what’s fueling your risk and suggest personalized steps to reduce the chances of stones in the future.
What should you know about vitamin supplements and kidney stone risk?
Some vitamin supplements can actually bump up your risk for kidney stones, especially if you’re already prone to them. For example, high doses of vitamin C (like the kind in some over-the-counter supplements) can raise oxalate levels in the urine—a known contributor to certain types of stones. Similarly, taking too much calcium or vitamin D without medical guidance may also tip the balance.
If you’re considering supplements, it’s a good idea to check in with your healthcare provider (and possibly a dietitian) first. They can help you weigh the pros and cons based on your personal risk and any medical conditions. A tailored approach helps you get the nutrients you need—without fueling unwanted stone formation.
How does eating meat affect your risk for kidney stones?
Diet plays a bigger role in kidney stone risk than most people realize, and animal protein is a common culprit. If your doctor spies high uric acid in your urine or you’re prone to certain types of stones (like calcium oxalate or cystine), reducing meat may help.
Here’s why: Eating a lot of animal protein (think beef, poultry, pork, fish, or even the weekend’s wild game) can tip the body’s chemistry, raising uric acid levels and lowering substances that help keep stones from forming. This means:
- More uric acid for your kidneys to filter—potentially forming stones.
- Less citrate (a natural inhibitor of stones) hanging around.
- A higher acid load in your urine, which increases the odds of calcium oxalate stones.
If this sounds familiar, clinicians may advise cutting back—maybe eating meat just once daily or making servings smaller, depending on your current habits and stone history. For some, even reducing intake by a few meals each week can make a difference.
Plant-based protein sources don’t carry the same risks, so swapping in beans, lentils, or tofu (think: Meatless Monday or Tuesday) could be a helpful move.
What are low-oxalate foods, and who should watch their oxalate intake?
Some people, especially those with a history of calcium oxalate kidney stones, may need to pay attention to oxalate in their diet. Oxalate is a compound found in many plant foods. When urine oxalate levels climb too high, it can boost the odds of forming one of the most common types of kidney stones.
For most folks, there’s no need to strictly avoid oxalate. But if your doctor has measured high urine oxalate, adjusting your diet might help. Eating calcium-rich foods with meals can actually lower oxalate absorption—counterintuitive, but true. If that’s not enough, cutting back on foods that are especially high in oxalate may be recommended.
Foods very high in oxalate include:
- Spinach
- Rhubarb
- Almonds
- Beets
- Swiss chard
- Sweet potatoes
You don’t have to avoid all oxalate-containing foods—nearly every fruit, vegetable, grain, or nut has some! Instead, it’s usually about moderating the big offenders while still enjoying a wide variety of nutrient-rich foods. Your individual reasons for high oxalate—and the right dietary tweaks—are best discussed with your healthcare provider or a registered dietitian.
The right amount of calcium for kidney stone prevention
If you’ve ever wondered whether to cut back or ramp up your calcium to dodge kidney stones, the answer is a classic Goldilocks situation—getting it “just right” matters. Most adults should aim for about 1,000–1,200 mg of calcium per day (from foods rather than supplements unless told otherwise by your provider). Both low and excessive calcium intake can tip the scales against you: skimping may actually increase your stone risk, while overdoing supplements can backfire as well.
So, what’s the best way to hit your target?
- Prioritize food sources. Three to four servings of calcium-rich foods daily usually cover your bases.
- Low-salt options are best. High salt intake encourages calcium loss in urine, another reason to go easy on processed foods.
- Don’t forget non-dairy sources. Calcium isn’t just hiding in milk and cheese—leafy greens, canned salmon (with bones), tofu prepared with calcium, and fortified beverages like almond or soy milk all count.
If you avoid dairy, look for calcium-fortified plant-based milks (see Silk, Califia Farms, or Almond Breeze). But before reaching for supplements, check in with your doctor or dietitian to tailor the plan to your needs and minimize stone risk.
Getting your calcium in balance is one piece of the puzzle—let’s look at other factors that influence stone type and frequency.
Salt and Kidney Stones: Why Sodium Matters
Salt (sodium) isn’t just about flavor—your intake can directly impact your risk for certain types of kidney stones, especially if you’re already prone to them. Here’s why: when you eat more salt, your kidneys tend to dump extra calcium (and sometimes cystine) into your urine. That excess can crystalize and form stones. So, dialing back on sodium is a well-established way to help prevent stone formation.
The CDC and most health authorities suggest keeping your sodium intake under 2,300 mg per day—that’s about one teaspoon of table salt. But many people get far more, mostly from store-bought and restaurant foods rather than what they sprinkle at the table.
Common high-salt offenders include:
- Cheeses (all varieties—think feta, cheddar, American, and even cottage)
- Processed and cured meats like cold cuts, bacon, ham, hot dogs, sausages, and salami
- Most frozen meals and ready-to-eat foods
- Canned soups, chili, and vegetables
- Breads, bagels, rolls, and bakery treats—not as salty per bite, but eaten often
- Salty snacks: tortilla chips, pretzels, salted nuts, crackers
- Bottled sauces, salad dressings, and marinades (hello, soy sauce)
- Pickles, olives, sauerkraut, and other preserved veggies
- Mixed dishes—think pizza, casseroles, lasagna, and fast-food combos
- Breakfast cereals (some brands sneak in surprising amounts of salt)
- Condiments (ketchup, mustard, some spice blends)
If you’re watching your salt, it can help to check labels, cook at home with fresh ingredients, and season food with herbs, spices, or citrus instead. A few simple swaps can make a real difference for your kidneys.
Can medications or supplements raise your risk?
Yes—some medications, along with calcium or vitamin C supplements, can tip the balance. For example, taking high-dose vitamin C may increase oxalate in your urine, while extra calcium (especially in pill form) might contribute to stone formation in those already prone. Certain diuretics, antacids, and even topiramate (a medication sometimes used for migraines or seizures) are also on the list of potential culprits.
If you’re concerned, let your healthcare provider know about everything you take—including over-the-counter vitamins or herbal products. Don’t make changes or stop prescriptions without their input, but keep them in the loop so they can tailor prevention strategies to your specific risks.
How animal protein impacts kidney stone risk
Eating a lot of animal protein—think beef, chicken, pork, or fish—can make your urine more acidic. This acidic environment favors the development of certain kinds of stones, especially calcium oxalate and uric acid stones. The way the body breaks down meat also leads to higher uric acid levels, which further increases your chances of forming both calcium and uric acid stones.
If you’re already at higher risk for stones, these dietary habits may tip the scale, so moderation and balance are important.
How does sodium (salt) intake influence kidney stone risk?
While calcium often gets the spotlight, sodium (salt) in your diet quietly plays a big role in kidney stone formation—especially when it comes to the most common type: calcium stones.
Here’s the crux: when you consume a lot of salt, your kidneys have to get rid of the extra sodium through your urine. This process pulls more calcium along with it into the urine, bumping up your chances for stones. In short:
- More salt = more calcium excreted in urine
- That extra urinary calcium means a higher risk your body will form stones
Interestingly, most specialists now caution against slashing dietary calcium (since too little can harm your bones and sometimes increase stone risk). Instead, they recommend keeping sodium intake in check as a practical way to lower how much calcium winds up in your urine.
So: if you’re aiming to cut your kidney stone risk, focusing on reducing salt—rather than calcium—may be a more effective move. Try easing up on processed foods, canned soups, restaurant meals, and salty snacks, all of which can sneak in surprising amounts of sodium.
Obesity can increase the risk of developing kidney stones. Research from sources like the Mayo Clinic and Cleveland Clinic highlights that being overweight may alter the chemical balance in the urine—particularly the amount of acid—making it easier for certain types of stones to form. In particular, obesity has been linked to higher levels of substances like calcium and uric acid in the urine, both of which can contribute to stone growth.
Weight gain and metabolic changes also seem to make stone formation more likely, especially in those already at risk. This means that maintaining a healthy weight (through diet, exercise, and regular healthcare checkups) can be one way to help lower your odds of having kidney stones.
How bowel conditions increase kidney stone risk
People with certain bowel conditions—like Crohn’s disease, ulcerative colitis, or those who’ve had intestinal surgeries (for example, gastric bypass)—face a higher risk for kidney stones, especially calcium oxalate stones. Here’s why:
- Chronic diarrhea, common in these conditions, causes the body to lose more fluids, which leads to less urine production. This “low flow” gives minerals and salts a better shot at sticking together and forming stones.
- At the same time, these bowel issues can change how the gut absorbs nutrients. Specifically, the intestine may soak up more oxalate from food. That extra oxalate then gets passed into the urine, bumping up the odds of crystals forming there.
So, both lower urine volume and higher oxalate levels become a “double whammy” for kidney stone risk in folks with these medical backgrounds.
The most common types of kidney stones
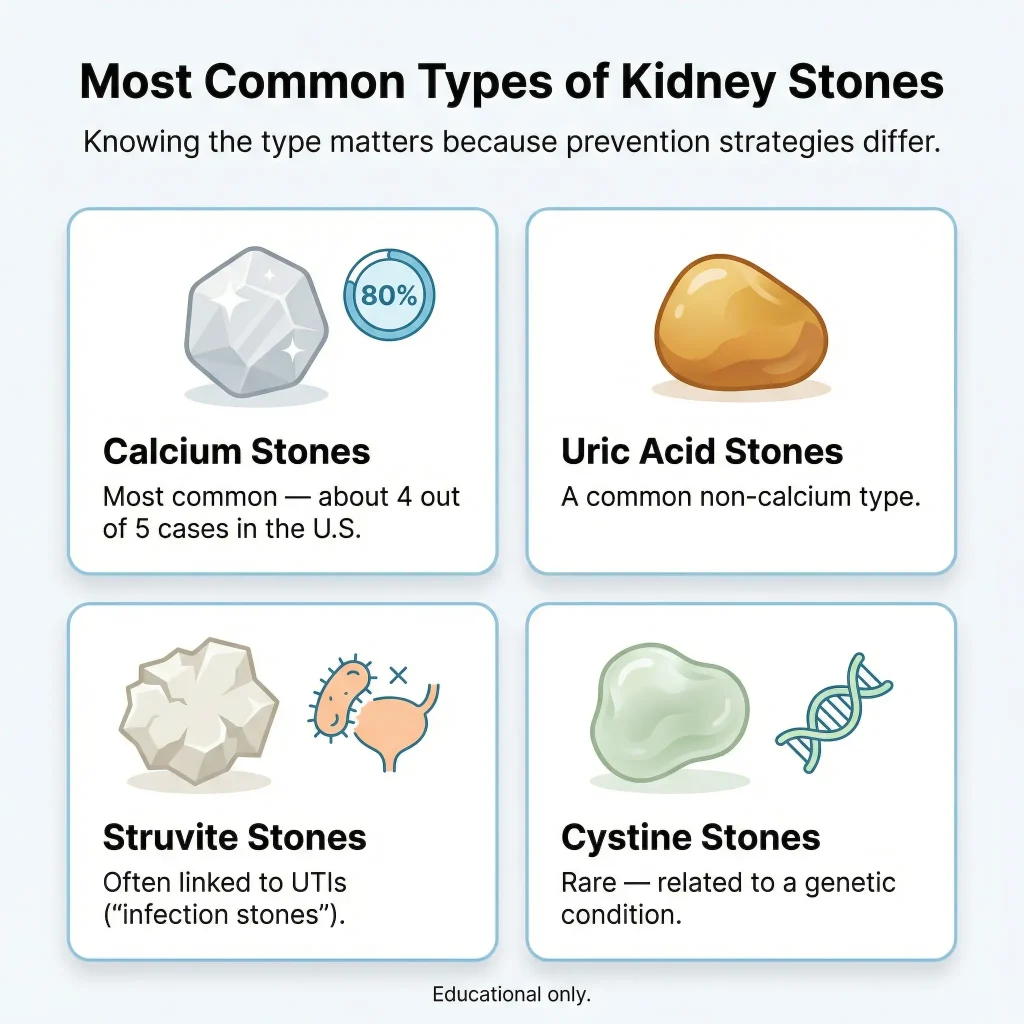
Knowing the type matters because prevention strategies differ.
American Kidney Fund (AKF) explains there are several types, including:
- Calcium stones (the most common; AKF notes they account for 4 out of 5 kidney stone cases in the U.S.)
- Uric acid stones
- Struvite (“infection”) stones linked to UTIs
- Cystine stones (rare, related to a genetic condition)
More about struvite (infection) stones
Struvite stones, sometimes called “infection stones,” make up about 10 percent of all kidney stones. These are typically linked to chronic urinary tract infections (UTIs). Certain bacteria can make urine less acidic (more alkaline), and in this environment, magnesium ammonium phosphate (struvite) stones can form—often quickly and sometimes growing quite large with branching shapes.
People at higher risk for struvite stones include those who have frequent or long-term urinary tract infections, individuals with long-term tubes (catheters) in their kidneys or bladders, and those with poor bladder emptying due to neurologic conditions like paralysis, multiple sclerosis, or spina bifida.
Understanding which type of stone you have matters, since prevention and treatment strategies differ.
What is a staghorn stone and how does it form?
Staghorn stones are a specific—and especially dramatic—type of kidney stone that can take up much of the space within the kidney, growing into branching shapes that resemble a stag’s antlers. These stones most commonly develop as struvite (“infection”) stones, which are linked to chronic or repeated urinary tract infections (UTIs) with certain bacteria.
Unlike smaller stones that make their presence known with sharp pain, staghorn stones may quietly expand over time and, surprisingly, often cause little to no pain at first. However, their sheer size and structure can seriously impact kidney function, even if urine flow isn’t completely blocked.
Key points about staghorn stones:
- Typically associated with recurrent UTIs.
- Most are struvite stones (as highlighted by the American Kidney Fund).
- They may not always cause symptoms until they’ve significantly affected the kidney.
- Can lead to long-term kidney damage if untreated.
Because they can develop silently and pose lasting risks, staghorn stones almost always require medical attention for removal and prevention of further kidney problems.
How common are kidney stones in the U.S.?
That’s why this topic is so heavily searched—and why prevention matters after the first stone.
How kidney stones are diagnosed
What your healthcare provider might ask about your history
To figure out your risk of more stones (and to fine-tune prevention), your clinician will ask questions about:
- Your personal stone history — Have you had kidney stones before? If so, how many times?
- Family history — Does anyone in your family have a history of kidney stones?
- Underlying health conditions — Do you have conditions like gout, diabetes, or digestive issues such as frequent diarrhea that are linked to higher stone risk?
- Dietary habits — What does your typical diet look like? Are there foods you eat that might increase your risk (like a lot of salt, animal protein, or high-oxalate foods)? Are you possibly missing protective foods, or might you not be drinking enough water?
This thorough review of your medical, family, and dietary background helps your provider assess how likely you are to develop more stones and guides what to check for next.
Urine and blood tests
NIDDK notes:
- urine tests can show minerals that form stones
- urinalysis can show blood, and white blood cells/bacteria may suggest a UTI
- blood tests can show mineral levels that contribute to stone formation
In practice, this means your clinician may collect both blood and urine samples after your history and physical exam. Blood tests can help uncover underlying medical conditions that might be causing your stones. Urine testing plays several roles: it can check for signs of infection, such as bacteria or white blood cells, and may also detect crystals typical of different stone types.
If you’re considered at higher risk for recurrent stones, your provider might recommend a 24-hour urine collection. This test measures the levels of various stone-forming substances in your urine throughout an entire day. The results can help tailor dietary advice or recommend specific medications to prevent future stones—an important step if this isn’t your first kidney stone rodeo.
Imaging
NIDDK explains imaging is used to find stones and can also show contributing problems like a blockage; abdominal x-rays can sometimes show stone location (though not all stones are visible on x-ray).
Mayo Clinic notes imaging tests (including CT) can show stones in the urinary tract.
If you have had stones before, clinicians may review any recent x-rays or order new ones to check for current stones or see if any have grown or moved. Imaging tests might also be repeated over time, especially if you have new symptoms like pain, visible blood in your urine, or recurrent infections. This helps your care team track the size and location of stones and guide further treatment.
Kidney stone treatment (what depends on size and symptoms)
NIDDK explains treatment is based on stone size, location, and type.
If the stone is small
NIDDK notes small stones may pass without treatment; a clinician may advise plenty of liquids (if appropriate) and may prescribe pain medicine.
If you pass a stone, clinicians may ask you to catch it so it can be tested to determine the type.
If the stone is large, blocking urine flow, or pain is severe
NIDDK states larger stones or stones that block the urinary tract or cause great pain may need urgent treatment—and if you are vomiting and dehydrated you may need hospital-level fluids through an IV.
Mayo Clinic similarly notes stones that are too large to pass may need more extensive treatment, and discusses procedures such as shock wave lithotripsy.
What if the stone won’t pass?
If a stone in the ureter does not pass in a reasonable time, or if it is causing significant pain, infection, or blocking the flow of urine, you may need surgery to remove it. Your care team will consider factors like the stone’s size, location, and any complications before recommending a procedure. In some cases, minimally invasive options can be used; in others, more traditional surgery may be necessary.
Getting prompt treatment is especially important if there are signs of infection (such as fever, chills, or difficulty urinating), as untreated blockages can lead to serious complications.
Can kidney stones cause kidney damage?
While most kidney stones won’t leave lasting harm, complications can arise if a stone leads to repeated infections or blocks the flow of urine for an extended period. According to NIDDK and Mayo Clinic, ongoing obstruction or untreated infections can eventually cause deterioration in kidney function. In rare cases—especially if a blockage isn’t relieved—there’s a risk that part or all of a kidney could stop working properly. Luckily, with timely diagnosis and appropriate care, permanent damage is uncommon.
What to expect after common procedures (SWL and URS)
Recovery after kidney stone removal depends on the approach, but most people bounce back fairly quickly.
For shock wave lithotripsy (SWL)—where sound waves break up the stone so it can pass more easily—you’ll often head home the same day. Many people are back to usual activities within a couple of days. You might be given a strainer to catch any stone fragments that pass in your urine, since your clinician will likely want to analyze these pieces to help guide future prevention.
Ureteroscopy (URS)—which uses a tiny scope to find and remove or break up stones—also usually lets you go home the same day. Most people are up and moving within 2-3 days. If a stent (a soft tube to keep the urine flowing) is placed, it generally comes out within a week or so. Some stents have a visible string, so you can remove them yourself, otherwise your healthcare provider will take care of it. It’s important not to delay removing the stent as directed—leaving it in too long can lead to infection or even permanent kidney damage.
Most people feel steadily better in the days after either routine procedure, but call your clinician promptly for high fever, trouble passing urine, or persistent severe pain.
What is a ureteral stent, and why might you need one after kidney stone removal?
Sometimes after removing a kidney stone (especially if it was large, tricky, or needed to be broken up), your urologist may place a ureteral stent. This is a thin, flexible tube that sits inside your urinary tract—specifically, stretching from the kidney to the bladder—to help keep the ureter open and allow urine to drain freely while the area heals.
Key points about ureteral stents:
- The stent is entirely internal, so you won’t have to deal with any external bags or tubes.
- Its main role is to prevent swelling or spasms from blocking urine flow after the stone (or fragments) have been taken out, reducing discomfort and complications.
- Most people recover quickly after stone removal with a stent in place and can usually get back to normal routines in a few days.
- The stent usually stays in for just a short period—often about 4 to 10 days. Sometimes, a small string is attached to make stent removal easier (and your provider will explain if you’ll need to pull it out yourself).
It’s crucial to have the stent removed when your urologist recommends it—leaving it in too long can increase the risk of infection or, rarely, kidney problems. If you ever have questions about your stent or symptoms while it’s in place, reach out to your medical team promptly.
What is ureteroscopy (URS) and how is it used to treat kidney stones?
If a kidney stone is too large to pass on its own or causing persistent symptoms, one common intervention is ureteroscopy (URS). URS is a minimally invasive procedure where a urologist guides a thin, flexible telescope (called a ureteroscope) through the urinary tract—starting at the bladder and advancing up the ureter to the kidney. This approach avoids the need for any external incisions.
The choice of instrument depends on the stone’s location:
- Rigid ureteroscopes are often used for stones lower down, near the bladder.
- Flexible ureteroscopes can reach stones higher up, including those lodged in the upper ureter or within the kidney itself.
Once the stone is directly visualized, smaller stones can often be captured and removed with a tiny basket-like tool. For larger stones, a laser (or other energy source) is used to break the stone into fragments, which are then removed or allowed to pass naturally.
After stone removal, it’s common for a urologist to place a temporary stent—a small internal plastic tube that helps keep the ureter open and allows urine to flow freely from kidney to bladder while the area heals. Unlike a catheter, a stent sits entirely inside the body and doesn’t require any external bags.
Recovery after URS is usually quick: many people go home the same day and return to routine activities within a couple of days. If a stent is placed, your healthcare team will give clear instructions for when and how it will be removed—sometimes with a simple office visit, or occasionally, you may be able to remove it yourself if given a special string. It’s crucial to follow these instructions, since leaving a stent in too long can increase the risk of infection or kidney problems.
Possible Side Effects and Complications of Shock Wave Lithotripsy
While shock wave lithotripsy (SWL) is commonly used and generally considered safe, it isn’t completely free of side effects. According to NIDDK and Mayo Clinic, some people may notice blood in the urine for a short time after the procedure, which is a typical and temporary finding.
Most of the resulting stone fragments tend to pass without much trouble. However, larger pieces may sometimes get stuck in the ureter (the tube connecting the kidney to the bladder). If this happens, it can trigger renewed pain and may require additional treatments or procedures to remove the fragments. Rarely, there can be other issues like bruising around the treated area or infection that needs medical attention.
If you experience severe pain, fever, or trouble urinating after lithotripsy, it’s important to check in with your clinician, as these can signal complications that need prompt care.
Managing kidney stones when you also have diabetes or heart conditions
Balancing kidney stone prevention with other health conditions—like diabetes or heart problems—often means you’re in luck: the core habits that help your heart and blood sugar also tend to keep stones at bay.
- Diet overlap: The classic “heart-healthy” diet promoted by organizations like the American Heart Association—think plenty of fresh produce, less salt, and a moderate approach to animal protein—also reduces stone risk in most people.
- Weight matters: Maintaining a healthy weight can lower your risk for both diabetes and kidney stones, and can help your overall kidney function.
- Personalization counts: Since each person’s needs are different, your clinician or a registered dietitian can help you adapt these recommendations to your individual health goals—especially if you have dietary restrictions for blood sugar or heart health reasons.
Bottom line: strategies that protect your heart and keep your diabetes in check often pull double duty in reducing stone risk, too.
What to expect during and after a PCNL procedure
For stones that are too large to pass on their own, a more advanced approach called percutaneous nephrolithotomy (PCNL) may be recommended. This procedure is often considered the gold standard for removing larger kidney stones.
PCNL is typically performed under general anesthesia. A urologist makes a small incision—about half an inch—on your back or side, creating a direct pathway to the kidney. A specialized telescope (nephroscope) is inserted, allowing the physician to locate and break up the stone. Uniquely, the technique also lets them suction out stone fragments right then and there, which is why it’s especially effective for bigger stones.
After the procedure, a drainage tube may be placed temporarily in your kidney. This allows urine to exit safely and helps control any possible bleeding. Usually, the tube stays in place for a day or two, and you’ll likely remain in the hospital overnight for monitoring and recovery.
Before discharge, imaging (like an X-ray) may be done to check for any remaining stone pieces. If fragments are still present, your doctor may go back in with a scope to remove them. Most people can return to normal routines within one to two weeks, although your care team will provide detailed recovery instructions tailored to your situation.
Why is PCNL considered the best treatment for large kidney stones?
For kidney stones that are too large to pass on their own, percutaneous nephrolithotomy (PCNL) is often considered the top treatment option. Mayo Clinic describes PCNL as a minimally invasive surgical approach: under general anesthesia, a small incision (about half an inch) is made in the back or side to access the kidney directly. Through this incision, a rigid scope is inserted, allowing the clinician to reach the stone.
The key advantage of PCNL is its ability to both break up and remove stone fragments in one procedure. Specialized instruments are used to shatter the stone, and then suction is applied to clear out the pieces—meaning large stones can be dealt with efficiently without the need for multiple procedures. This direct access and efficient stone removal make PCNL the most effective choice, especially when stones are causing blockage, repeated infections, or are simply too big for less invasive options.
For kidney stones that are too large to pass on their own—or can’t be treated effectively with less invasive methods—clinicians may recommend a procedure called percutaneous nephrolithotomy (often shortened to PCNL).
Mayo Clinic and NIDDK outline PCNL as a minimally invasive surgery performed under general anesthesia. Here’s what typically happens:
- A small incision (about half an inch) is made in your back or side.
- Using this entry point, the surgeon guides a thin, rigid telescope (called a nephroscope) directly into the part of the kidney where the stone is sitting.
- Specialized tools are then used through the nephroscope to break the stone into smaller pieces. Because PCNL allows for suctioning out stone fragments, it’s particularly useful for large stones.
- After the main procedure, a temporary drainage tube may be left in the kidney to help urine flow and reduce any risk of bleeding. This tube generally stays in place overnight, or for a few days, depending on your recovery.
- Before you leave the hospital (usually after a brief stay), imaging such as an X-ray may be done to check for any leftover stone fragments. If remnants remain, the clinician may advise a second, similar procedure to remove them.
Most people can get back to their usual activities within one to two weeks after PCNL.
How to prevent kidney stones
Prevention becomes much more targeted once the stone type is known. NIDDK emphasizes prevention is easier when you know what caused your previous stone.
Hydration is the foundation
NIDDK says drinking enough liquids each day is “the best way” to help prevent most stones because it keeps urine diluted and flushes away minerals.
But how much is enough? In general, aim for at least 3 liters (about 3 quarts, or ten 10-ounce glasses) of fluid a day—unless your healthcare provider tells you otherwise. This is the amount typically recommended to help lower the risk of forming new stones. All fluids count toward this goal, but it’s wise to focus on no-calorie or low-calorie drinks, and to limit sugary sodas and alcoholic beverages.
If you want to be precise, try measuring your daily fluid intake with a household measuring cup, or use bottles and cans with fluid ounces clearly listed. Track what you drink over a day or two, and add up the ounces—your target is to produce at least 2.5 liters (about 85 ounces) of urine per day. Keeping a log (even a quick note on your phone) can be surprisingly helpful for hitting this target.
NIDDK adds that if you live/work/exercise in hot weather, you may need more fluids to replace what you lose through sweat.
That’s particularly relevant in Houston summers—people can become dehydrated faster than they realize.
Special note: People who form cystine stones may need to drink even more—sometimes up to 4 liters a day—to help reduce stone-forming substances in their urine. Always follow your healthcare provider’s advice for your unique situation.
Citrus can help (when appropriate)
NIDDK notes some studies suggest citrus drinks like lemonade or orange juice may help prevent stones because they contain citrate, which can stop crystals from turning into stones.
Diet tweaks that make a difference
Stay well hydrated:
Drinking enough fluids each day is one of the best ways to lower your risk of developing new stones. For most people, this means aiming for at least 3 liters (about 3 quarts) of liquid daily—roughly ten 10-ounce glasses. If you’re sweating more due to Houston heat or exercise, you’ll need to replace what you lose. All fluids count, but it’s best to focus on water or other low- or no-calorie drinks. Keeping a daily log (even just jotting down bottle sizes and how many you drink) can help you track your intake and make sure you’re on target.
People who form cystine stones may need even more—often up to 4 liters a day—to help flush out those specific compounds.
Cut back on salt:
Too much sodium can raise calcium and cystine in the urine, upping your stone risk. The CDC recommends no more than 2,300 mg of salt per day. Watch out for salty staples like cheese, cured meats (think deli meats, sausages, and hot dogs), canned soups, breads, chips, and bottled dressings or sauces. Even some breakfast cereals can be surprisingly high in salt.
Get the right amount of calcium (not too much, not too little):
Don’t overdo it with calcium supplements unless your doctor advises them—excess calcium can backfire. On the flip side, too little calcium can also be a problem. Most people can meet their needs with three or four servings of calcium-rich foods daily, like dairy or calcium-fortified non-dairy alternatives. Aim for low-salt options when you can.
Load up on fruits and veggies:
Aim for at least five servings a day. Fruits and vegetables provide potassium, magnesium, fiber, antioxidants, and citrate (the same helpful compound found in citrus), all of which can help block stone formation.
Watch oxalate if needed:
If you’re someone with high urine oxalate, certain foods—like spinach, rhubarb, and almonds—are especially high in oxalate and may need to be limited. Pairing calcium-rich foods with meals can help lower oxalate absorption. Most people don’t need to cut out oxalate completely; your doctor or dietitian can help tailor recommendations.
Consider animal protein:
If your urine uric acid is high, your clinician might suggest eating less meat, fish, poultry, or seafood. Sometimes, this means cutting back to once a day or a few times a week, depending on your current habits and your stone type.
These dietary steps, along with staying well hydrated and considering citrus drinks, can help tip the odds in your favor for preventing future stones.
Medications may be used for prevention
NIDDK lists examples of preventive medicines based on stone type (e.g., potassium citrate for some stone types; antibiotics for struvite stones).
Common preventive medications
- Thiazide diuretics: Used for people with calcium stones and high calcium in their urine. Thiazides help the kidneys reabsorb calcium so less ends up in the urine. These work best when you also limit salt intake, since high sodium can counteract their effect.
- Potassium citrate: Often prescribed for those with calcium stones and low urinary citrate, or for uric acid and cystine stones. Potassium citrate makes urine less acidic (more alkaline), which helps prevent uric acid and cystine stones and raises citrate levels to protect against calcium stones.
- Allopurinol: Frequently used for people with gout or high uric acid. It lowers uric acid levels in both blood and urine, and may help prevent calcium and uric acid stones.
- Acetohydroxamic acid (AHA): Sometimes recommended for people who keep forming struvite (infection) stones, especially if caused by frequent UTIs. AHA changes the urine chemistry to make it less hospitable for these stones to form, but complete removal of stones and infection control are still key.
- Cystine-binding thiol drugs: Medications like d-penicillamine or tiopronin are used in rare cases for people with cystine stones, especially if other measures like increased fluids and potassium citrate haven’t worked. These drugs bind cystine, making it less likely to form crystals.
A note on supplements
Be cautious with vitamin supplements—some can raise your risk for kidney stones. It’s wise to discuss any supplements with your healthcare provider or a dietitian before starting them.
What if you keep getting kidney stones, even with treatment?
It’s possible for kidney stones to recur, even if you’ve already had procedures, adjusted your diet, or are taking prescribed medicines. If you find yourself forming new stones despite these steps, it’s important not to get discouraged.
The next move: talk with your healthcare provider about a more tailored prevention plan. Some people need additional urine or blood tests to look for underlying causes, such as high levels of certain minerals or unrecognized medical conditions. Your clinician may recommend:
- Reviewing your current medications and supplements to spot anything that could contribute to stones
- Meeting with a registered dietitian (especially helpful for complex dietary triggers)
- Increasing or adjusting fluid intake, based on your individual risk factors and environment
- Exploring further prevention medications, or fine-tuning your existing regimen
For some, a nephrologist or urologist can help dig deeper into stubborn cases. The key is to keep the conversation going—more detailed testing and a personalized approach can help lower your chances of repeat stones.
Why follow-up matters after a kidney stone
Following up with your healthcare provider isn’t just a box to check—it’s key to making sure your recovery stays on track and prevents future stones.
- Fine-tuning your treatment: Your clinician might repeat blood tests, urine analyses, or even another 24-hour urine collection to see if the measures you’ve taken (like medication or dietary changes) are actually working.
- Catching new stones early: For those prone to recurrent stones, occasional imaging—such as X-rays or ultrasounds—helps spot any new trouble before symptoms kick in.
- Managing medication and side effects: Your healthcare provider will also want to check for side effects from your medications and adjust your regimen as needed to keep you feeling your best.
In short, regular monitoring can help avoid surprises, ensure your kidney stone plan is actually effective, and help you and your clinician make smart adjustments as needed.
Warning symptoms that shouldn’t wait

NIDDK explicitly advises seeing a healthcare professional right away for symptoms that may mean a kidney stone or a more serious condition.
Get evaluated urgently if you have:
- Fever or chills (possible infection complication)
- Persistent vomiting or signs of dehydration (NIDDK notes vomiting/dehydration may require IV fluids)
- Inability to urinate or only passing a small amount
- Pain that is escalating, unmanageable, or paired with significant weakness/lightheadedness
- A known stone with worsening symptoms, especially with urinary changes
If you’re in Houston and your symptoms fall into the “warning symptoms that shouldn’t wait” category—especially severe flank pain, vomiting/dehydration, or fever/chills—it’s reasonable to get checked promptly.
Post Oak ER states it is open 24/7 with board-certified physicians, and they highlight advanced on-site diagnostics including CT, X-ray, ultrasound, and laboratory services.
They also note they’re located just off San Felipe St. near The Galleria and Uptown Park, and that patients across Houston—from Uptown to the Energy Corridor, and from Westchase, Midtown, and the Heights—reach them easily.
Frequently Asked Questions
How long does it take to pass a kidney stone?
It varies by stone size, location, and your anatomy. Clinicians typically decide next steps based on symptoms, stone size/location, and whether urine flow is blocked.
Can I prevent stones from coming back?
Yes—especially once the stone type is known. NIDDK emphasizes hydration as a primary prevention step and notes diet/medication changes may be recommended based on your stone type.
Is blood in urine always a kidney stone?
No. NIDDK lists blood in urine as a kidney stone symptom, but blood in urine can have other causes too—which is why evaluation matters, particularly if it persists or comes with fever or severe pain.
Do lemonade or citrus drinks help?
NIDDK notes citrus drinks may help prevent stones because citrate can prevent crystals from becoming stones (not appropriate for everyone—your clinician can advise based on your case).