If you’re searching kidney failure, you’re probably trying to answer one urgent question: How serious is this—and what should I do right now?
Here’s the clearest way to think about it: kidney failure isn’t one single scenario. Some people develop kidney failure slowly (advanced chronic kidney disease), while others develop it suddenly (acute kidney injury). The “right next step” depends on which situation you’re in and how you’re feeling.
This guide explains what kidney failure means, the most common symptoms, why it happens, what treatment typically looks like, and warning symptoms that shouldn’t wait.
Educational only. Not medical advice or a diagnosis.
What is kidney failure?
Kidney failure as the last stage of CKD (ESRD/ESKD)
The National Kidney Foundation explains that kidney failure (also called ESRD) is the last stage of chronic kidney disease, and treatment typically involves dialysis or a kidney transplant.
Mayo Clinic similarly describes end-stage renal disease (end-stage kidney disease / kidney failure) as occurring when chronic kidney disease reaches an advanced state and the kidneys can no longer meet the body’s needs.
Kidney failure that happens suddenly (acute kidney injury)
Not all kidney failure is gradual. NKF explains that acute kidney injury (AKI) occurs when the kidneys suddenly lose their ability to filter waste—often developing within hours or days—and it replaces the older term “acute renal failure.”
What tests are used to diagnose kidney failure?
If a healthcare provider suspects kidney failure, several tests can help confirm what’s going on and how severe the problem is:
- eGFR (estimated glomerular filtration rate): This blood test measures how well your kidneys are filtering waste by checking your creatinine level, then factoring in your age and sex to estimate overall kidney function. According to the National Kidney Foundation and Mayo Clinic, eGFR is typically the main number used to monitor kidney health.
- uACR (urine albumin-to-creatinine ratio): This urine test checks for protein (albumin) in your urine—a sign that your kidneys’ filters are leaking and could be damaged. Persistently high levels are a red flag for chronic kidney issues.
- Kidney biopsy: If the root cause of kidney disease isn’t clear, doctors may use a biopsy—a small tissue sample from the kidney—to look for specific damage under the microscope. This test is less common but helps guide treatment in complex cases.
These tools, paired with your medical history and symptoms, help doctors map out the best plan for your care.”
Kidney failure symptoms
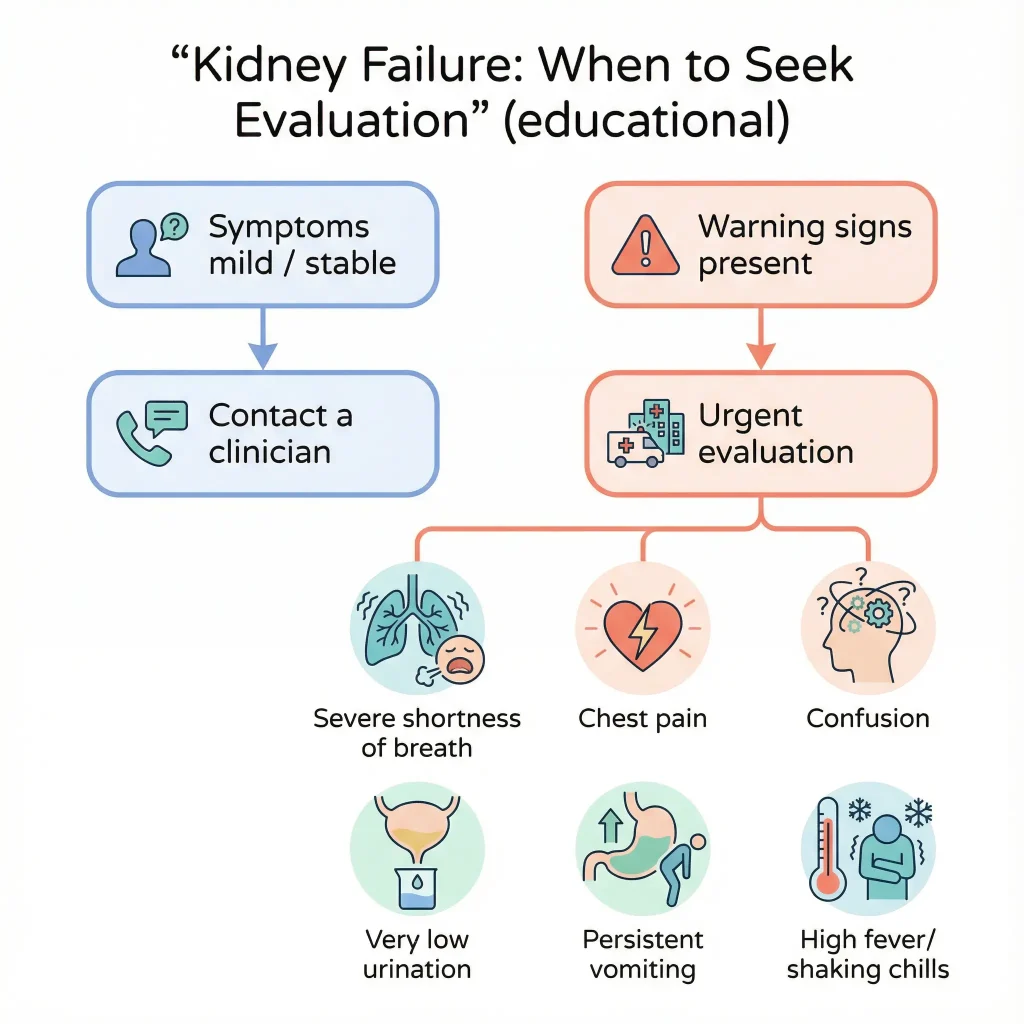
Symptoms can vary based on whether the issue is acute or chronic, but common warning patterns include:
- Swelling in legs/feet/face (fluid retention)
- Shortness of breath (can happen when fluid overload affects the lungs)
- Marked fatigue, weakness, or confusion
- Very little urination (or sudden major change from your baseline)
- Nausea/vomiting or inability to keep fluids down
Cleveland Clinic notes kidney failure may be acute or chronic and highlights that end-stage kidney disease is deadly without treatment.
What causes kidney failure?
Chronic (slowly progressive) causes
When kidney failure develops gradually, it is usually the result of long-standing kidney damage (advanced CKD). NKF’s kidney failure overview frames kidney failure as the last stage of CKD.
Acute causes
When kidney function drops suddenly, common contributors can include severe illness, dehydration/low blood flow to kidneys, medication toxicity, obstruction, or serious infection—depending on the person and situation.
NKF emphasizes the defining feature of AKI is the sudden loss of filtering ability.
Mayo Clinic notes acute kidney injury can lead to serious complications, including death, and in some cases can contribute to end-stage kidney disease.
Can you die suddenly from kidney failure?
People usually mean one of these scenarios:
Untreated end-stage kidney disease
Cleveland Clinic notes end-stage kidney disease is deadly without treatment and states that without treatment, survival may be days to weeks (varies by the individual).
This is why dialysis/transplant planning is so important before kidney function reaches a crisis point.
Acute kidney injury during a medical emergency
AKI can develop quickly, and Mayo Clinic notes it can cause kidneys to stop working and can be fatal.
When AKI is part of a bigger emergency—severe dehydration, sepsis, major infection—waiting at home can be dangerous.
Sepsis (infection-triggered organ failure)
Sepsis can begin from infections that often start in the urinary tract, and without fast treatment can rapidly progress to tissue damage, organ failure, and death.
This is one reason kidney-related infections should never be treated casually when symptoms are escalating.
How is kidney failure treated?
Treatment depends on the cause and stage—but the “big picture” options are consistent across major kidney foundations.
Treat the cause (especially in AKI)
In acute kidney injury, the immediate goal is to stabilize the body and correct what is damaging kidney function (fluids, infection management, stopping harmful meds, relieving obstruction, etc.).
Dialysis and transplant (for ESRD/ESKD)
NKF states that when kidneys fail (ESRD), treatment is typically dialysis or kidney transplant.
What is medical management if I choose not to get treatment for kidney failure?
Not everyone opts for dialysis or transplant when facing end-stage kidney failure. In these situations, a path called medical management (sometimes called conservative, supportive, or comfort-focused care) may be chosen instead.
Medical management focuses on relieving symptoms and supporting quality of life without trying to replace kidney function. Your healthcare team—often including your primary care provider, nephrologist, and sometimes a palliative care specialist—works closely with you to ease symptoms like pain, nausea, itching, and shortness of breath. They’ll often adjust medications, recommend lifestyle changes, and help you avoid complications such as infections or fluid overload.
How long someone lives with only medical management is highly individual and varies widely. Honest, ongoing conversations with your care team are essential to plan ahead, address your priorities, and ensure comfort as much as possible. This approach is about maximizing well-being, respecting personal choices, and providing support both for you and your loved ones during a challenging time.
Resources and Support for People Living with Kidney Failure
Managing kidney failure is no small feat, and it’s completely normal to feel uncertain or overwhelmed as you navigate diagnosis, treatment decisions, and lifestyle changes. Fortunately, you don’t have to do it alone—there are practical resources and support systems ready to help.
Educational Support and Community Connections
- Patient support groups: Many hospitals and organizations (like the National Kidney Foundation and American Association of Kidney Patients) offer online communities and local meetings where you can share experiences and get advice from others in similar situations.
- Trusted information hubs: Reputable sites—including Mayo Clinic, Cleveland Clinic, and National Kidney Foundation—provide reliable, up-to-date education about symptoms, treatment options, and what to expect along your journey.
- Caregiver guidance: Family and friends play a key role. Encourage them to read about kidney failure, attend doctor’s visits if possible, and make use of caregiver-focused resources offered by major kidney organizations.
Navigating Treatment Decisions
- Checklists and guides: Preparing for dialysis, transplant consideration, or new medications can be daunting. The National Kidney Foundation’s “Dialysis Choices” guide and the Mayo Clinic’s patient materials give step-by-step advice on what questions to ask and how to plan.
- One-on-one support: Social workers, renal dietitians, and your nephrology care team can personalize guidance on everything from nutrition choices to managing side-effects and organizing daily routines.
Mental Health & Emotional Well-Being
- Coping resources: It’s normal to experience a range of emotions—from sadness and anxiety to frustration. Larger clinics typically have mental health counselors and social workers familiar with the unique challenges faced during kidney failure.
- Depression support: If you notice persistent low mood or trouble adjusting, let your care team know. Evidence-based treatments—including therapies, support groups, and sometimes medication—can make a real difference, and organizations like Mental Health America and the National Alliance on Mental Illness provide additional guidance.
Lifestyle and Nutrition Support
- Renal dietitians: These nutrition experts can help tailor meal plans suited to your stage of kidney disease, personal preferences, and lab results.
- Educational kitchen tools: The National Kidney Foundation’s “Kidney Kitchen” and Mayo Clinic’s renal nutrition pages offer recipes and practical tips for eating well with kidney disease.
Staying Informed and Finding More Help
- Webinars and workshops: Many kidney organizations and health systems offer regular educational events on topics ranging from dialysis to mental health and living well with chronic illness.
- Reliable resource directories: If you still have questions, consider browsing sections like the Cleveland Clinic or National Kidney Foundation’s online resource libraries for deeper dives into specific topics.
Remember, the path through kidney failure is unique for everyone, and reaching out for help—whether practical or emotional—can make the journey more manageable.
Adjusting to Life on Dialysis
Starting dialysis marks a significant change, and it’s perfectly normal for the process to feel daunting at first. Most people find there’s an adjustment period as you and your family get used to new routines—everything from scheduling treatments to managing daily activities and meals.
Here’s what you can expect as you begin dialysis:
- Learning the Treatment Options: Your care team will walk you through the main types of dialysis—hemodialysis or peritoneal dialysis—and help you choose the option that fits best with your lifestyle and health needs.
- Building Your Routine: Dialysis impacts your schedule, especially if you’re traveling to a center several times a week. Many patients find it helpful to set reminders, enlist family support, and communicate with their employer or school as needed.
- Adjustments at Home: There may be changes in your diet, fluid intake, and medications. Registered dietitians from organizations like the American Kidney Fund or National Kidney Foundation often provide practical tips to ease this transition.
- Emotional Ups and Downs: It’s common to experience a mix of relief, anxiety, or even sadness when starting dialysis. Support groups—either locally or online—can be invaluable resources for both patients and families.
Dialysis is a big shift, but you aren’t alone. Most people find that after the initial adjustment—usually a few weeks—they’re able to settle into a new “normal.” With good support, planning, and open communication with your healthcare team, managing dialysis becomes more routine over time.
Types of Dialysis
When kidneys can’t do their job, dialysis steps in to help filter out waste and extra fluid. There are two main forms of dialysis, each with a distinct approach:
- Hemodialysis:
This is the most recognized type. Your blood is circulated through a special machine that removes waste and balances fluid and electrolytes before returning it back to your body. Treatments are often done at a dialysis center, though in some cases, home hemodialysis may be an option. - Peritoneal Dialysis:
Instead of using a machine, this method uses the lining of your abdomen (the peritoneum) as a natural filter. A cleansing fluid is infused into your belly through a small tube. After it absorbs waste products, the fluid is drained and replaced on a set schedule. Peritoneal dialysis is usually performed at home, offering more flexibility for some patients.
Both approaches aim to maintain your body’s chemical balance and prevent build-up of dangerous toxins, either as a bridge to transplant or when long-term dialysis is needed.
What lifestyle changes and steps can support living with kidney failure?
Managing kidney failure is about stacking the odds in your favor—everyday choices matter. Along with medical treatments like dialysis or transplant, proactive self-care helps maintain the best possible quality of life.
Key recommendations include:
- Stick to treatment appointments. Attending every scheduled dialysis session is crucial, as is starting the conversation early about transplant options and referrals.
- Partner with specialists. Regular visits with your nephrologist (kidney doctor) help track how things are going. If you have diabetes, close monitoring—potentially with an endocrinologist—can be vital.
- Embrace a kidney-friendly diet. Consulting a registered dietitian is invaluable. They can help tailor an eating plan that fits your stage of kidney disease, personal preferences, and any dietary restrictions.
- Keep blood pressure in check. Taking any prescribed medications as directed, limiting sodium, and monitoring your numbers at home all play a role in reducing further kidney damage.
- Aim for steady blood sugar. For those with diabetes, diligent glucose management can slow the progression of kidney disease and help prevent complications.
- Move regularly. Even moderate activity—like walking most days—can boost energy, mood, and cardiovascular health.
- Limit or avoid tobacco and alcohol. Both can stress the kidneys and raise risks for other health problems, so cutting back is strongly advised.
Remember, the recipe is all about long-term consistency—not perfection. Consulting with your care team about changes, symptoms, or challenges can help fine-tune your plan and spot trouble early.
What should I eat with kidney failure?
Diet is a crucial part of managing kidney failure—and it often changes depending on your stage, your labs, and whether you’re on dialysis or have had a transplant.
When your kidneys aren’t filtering as they should, you may need to limit certain foods and fluids to avoid putting excess strain on your kidneys or letting waste build up in your blood. While dialysis takes over some of your kidneys’ work, it doesn’t do everything, so dietary choices still matter.
Here’s what to keep in mind:
- Fluid control: Depending on your dialysis plan and how much urine you’re making, you may need to limit fluids to prevent swelling, high blood pressure, or shortness of breath.
- Sodium: Cutting back on salt can help control blood pressure and reduce fluid overload.
- Potassium and phosphorus: Blood levels of these minerals often rise in kidney failure, so you may need to swap certain fruits, veggies, and dairy for lower-potassium and lower-phosphorus alternatives.
- Protein: Some people need more protein (especially if on dialysis), while others need to moderate it. Your care team will help you strike the right balance.
All the above should be tweaked with your nephrologist and, ideally, a registered dietitian well-versed in kidney disease. Your diet may shift over time based on your labs and which treatment you’re on.
A few resources worth exploring: The National Kidney Foundation and the Mayo Clinic offer meal planning guides and tips for managing your diet with kidney failure.
The role of a dietitian in kidney failure
Managing kidney failure isn’t just about medications and treatments—it’s also about what you eat and drink every day. Because kidney disease changes the way your body handles fluids, minerals, and nutrients, figuring out the right food choices can quickly become overwhelming.
That’s where a registered dietitian comes in. They translate the confusing nutrition “dos and don’ts” into a practical, personalized eating plan tailored to your stage of kidney disease, other medical conditions (like diabetes or high blood pressure), lab results, and even your favorite foods.
A dietitian’s guidance can help:
- Limit excess sodium, potassium, and phosphorus—which can build up to dangerous levels when kidneys aren’t working well
- Ensure you get enough calories and protein (but not too much) to maintain strength without overloading your kidneys
- Adjust your meal planning as your health needs or treatments change
Ultimately, working with a dietitian helps you navigate the grocery store (and real life), supports your overall health, and may help you feel better day-to-day—making nutrition an active part of your care, not just an afterthought.
Kidney transplant options: Deceased vs. living donors
For people with end-stage kidney disease, kidney transplant is often considered the definitive long-term treatment. There are two main types of kidney transplants, each with its own unique process and considerations:
- Deceased donor transplant: This option involves receiving a kidney from someone who has recently passed away. These kidneys come from organ donors who, through their or their families’ consent, have made their organs available to those in need. Wait times can be variable, as there are more people in need of a kidney than there are available organs, and matching for blood type and other factors is carefully managed by national organizations.
- Living donor transplant: In this scenario, a healthy individual—often a family member, friend, or sometimes an altruistic stranger—donates one of their kidneys. Living donor kidneys tend to function more quickly after transplant and often last longer than deceased donor kidneys. The evaluation process for both donor and recipient is thorough, but outcomes are generally excellent.
Both options have specific medical and logistical steps, but the ultimate goal is the same: restoring kidney function and quality of life. Deciding between them depends on personal situation, availability, and the recommendations from your kidney care team.
Coping with Kidney Failure: Navigating the Emotional and Physical Journey
Being told you have kidney failure is more than just a medical diagnosis—it’s a tidal wave of emotions, ranging from fear and frustration to sadness and overwhelm. All of these are absolutely normal reactions. No one sails through this alone, and connecting with supportive people—your healthcare team, family, friends, and perhaps others living with kidney disease—can make all the difference.
Caring for Your Body (and Mind) Through Treatment
To help you feel and function at your best, your doctors will likely recommend a comprehensive approach. Here are some key components most kidney foundations and organizations agree on:
- Stay on top of dialysis or transplant planning
Attend all scheduled dialysis sessions if prescribed, and speak with your care team early about evaluating your options for a kidney transplant. - Get specialized guidance
Regular visits with a nephrologist ensure your treatment plan is on track. A registered dietitian can tailor a kidney-friendly nutrition plan, which may help manage symptoms and energy levels. - Mind blood pressure and blood sugar
These two numbers matter—a lot. Keeping them in a healthy range (with medications and lifestyle, as needed) protects your heart and what’s left of your kidney function. For those with diabetes, coordinating care with an endocrinologist is often recommended. - Move your body
Regular activity—even light walking most days—can boost energy, lift mood, and help control blood pressure. - Minimize alcohol, avoid smoking and tobacco
Both substances put extra strain on your kidneys and can worsen complications. Your care team can provide resources and support for quitting if it’s challenging.
Emotional Health: Just as Important
Don’t underestimate the mental toll. Feelings of grief, anxiety, or anger are valid, and addressing them is part of the healing process. Consider:
- Speaking openly with your healthcare team about emotional struggles.
- Seeking counseling or joining a kidney disease support group.
- Connecting with loved ones and letting them support you.
Taking care of your mental health doesn’t just ease the emotional burden—it can improve physical outcomes, too. If you need more tailored support, resources from groups like the National Kidney Foundation or American Psychological Association can help guide your next steps.
Managing Depression and Mental Health with Kidney Disease
Coping with kidney disease isn’t just a physical challenge—it can weigh heavily on your mood and mental health, too. It’s common for people with chronic kidney issues to face sadness, anxiety, or depression along the way. But these feelings aren’t just “part of the package”—there are ways to manage and feel better.
Consider some practical strategies:
- Talk to your care team: Mention any mood changes, persistent sadness, trouble sleeping, appetite loss, or hopeless feelings to your doctor or nephrologist. Depression is common and highly treatable. Early conversation is key.
- Seek professional support: Therapy (like cognitive-behavioral therapy) can be enormously helpful. Some patients benefit from speaking with a psychologist, social worker, or support group—whether in-person or through organizations like the National Alliance on Mental Illness (NAMI) or Mental Health America.
- Medication: If depression is significant, antidepressant medications may be considered—your doctors can help select safe options given your kidney function.
- Stay connected: Reach out to family, friends, or peer groups for emotional support. Sharing your experience can make daily hurdles more manageable.
- Focus on small wins: Set realistic daily goals and routines. Gentle exercise, enjoyable activities, and mindfulness practices (like meditation) may also help improve mood and manage stress.
- Know you’re not alone: Depression is a medical condition, not a personal failure. Many people with kidney disease experience it, and getting help can make a world of difference.
If you’re struggling, don’t wait—support is available, and treatment works.
Estimating Kidney Transplant Wait Times
If you’re trying to figure out how long you might wait for a kidney transplant, there’s a helpful tool offered by the Scientific Registry of Transplant Recipients (SRTR). Their Kidney Transplant Waiting Times resource lets you see typical wait times for people with health backgrounds similar to yours, using the most recent national data (including both active and inactive time on the waitlist).
While the numbers aren’t exact predictions—every situation is unique—they provide a realistic ballpark estimate so you can prepare and plan accordingly. This can help you have more informed conversations with your care team and set expectations about the transplant process.
If you’re in Houston and you’re dealing with warning symptoms that shouldn’t wait, getting evaluated sooner is often the safer decision—especially if breathing, mental clarity, urination, or hydration are changing fast.
Post Oak ER states it is open 24/7 with board-certified emergency physicians and advanced on-site diagnostics, including CT, X-ray, and laboratory services.
They also note they are open 24/7 near The Galleria.

