If you’ve had a kidney stone before, you already know the real question is not just how to get through the pain. It is how to stop it from happening again. Prevention matters because kidney stones are common. The American Kidney Fund says over 1 in 10 men and about 1 in 14 women in the United States will have a kidney stone at least once in their lives.
The good news is that kidney stone prevention is not guesswork. The most useful strategies usually come down to hydration, targeted diet changes, and, for some people, medications based on the stone type and lab findings. NIDDK states that doctors help prevent kidney stones by having patients drink enough liquid, change what they eat, or take medicines.
Educational only. This is not medical advice or a diagnosis.
Why kidney stones form in the first place
Kidney stones form when certain substances in urine become concentrated enough to crystallize and stick together. NIDDK explains that kidney stones are linked to high levels of calcium, oxalate, and phosphorus in the urine, and its kidney-stone overview emphasizes causes, symptoms, diagnosis, prevention strategies, and treatment options.
That means prevention is usually about lowering the chance that urine becomes the right environment for crystals to build up. In practical terms, the biggest levers are usually enough fluid, better urine dilution, and, when needed, diet or medication changes tailored to the stone type.
Hydration is still the foundation
For most adults, the single most important prevention habit is drinking enough fluid. NIDDK says that unless you have kidney failure, you should usually drink six to eight, 8-ounce glasses of water a day, and it also states that drinking enough liquid each day is the best way to help prevent most kidney stones.
Why water matters
When urine is more diluted, stone-forming minerals are less likely to build up and crystallize. NIDDK’s prevention guidance specifically frames higher fluid intake as a way to help keep stones from forming again.
Hot weather changes the equation
NIDDK also notes that if you live, work, or exercise in hot weather, you may need more fluid to replace what you lose through sweat. That is especially relevant in Houston, where heat and humidity can quietly increase dehydration risk.
Diet changes can help — but they should be targeted
A lot of people want a simple “kidney stone diet,” but the honest answer is that prevention works best when it is matched to the kind of stone you form. NIDDK’s diet-and-nutrition guidance says diet can help prevent or relieve stones, and its treatment/prevention guidance says doctors may recommend changing what you eat to help prevent stones from coming back.
Sodium matters
High sodium intake can make kidney stone prevention harder, which is one reason clinicians often focus on salt intake when discussing prevention. NIDDK includes diet changes as a core part of prevention strategy, especially for people with repeat stones.
Protein, oxalate, and stone type matter
Not every person with stones needs the exact same food restrictions. Prevention is more precise when doctors know what the stone was made of and what your urine testing shows. NIDDK’s kidney-stone treatment page emphasizes that treatment and prevention depend on stone size, location, and type, and that prevention becomes easier once the stone type is known.
Citrus may help some people
Why stone type changes prevention advice
Not all kidney stones are the same, and prevention advice should not pretend they are. The American Kidney Fund explains that there are several major stone types, including:
- calcium stones (the most common, accounting for 4 out of 5 kidney stone cases in the U.S.)
- uric acid stones
- struvite stones linked to infection
- cystine stones, which are rare and genetic.
That matters because prevention differs:
- some people need more emphasis on hydration and sodium control
- some need stone-specific medication
- some need infection prevention if they form struvite stones.
Medications can help prevent stones in the right patients
If you keep forming stones, prevention may go beyond water and diet. NIDDK says doctors may prescribe medicines to help prevent stones, depending on the kind of stone and your overall situation.
NIDDK’s treatment page also notes that preventive medicines may be chosen based on stone type, and that this is one reason catching and analyzing a passed stone can be useful.
Important: this is not a DIY category. Preventive medication is something to review with a clinician after the stone type and risk profile are clearer.
Prevention is easier after the first stone is analyzed
One of the most practical things you can do after passing a stone is help identify what kind it was. NIDDK explains that treatment and prevention depend on stone type and that patients may be asked to catch the stone so it can be tested.
That information can make the prevention plan far more specific and useful than generic advice found online.
What actually helps most in real life
If you want the most realistic prevention checklist, it usually looks like this:
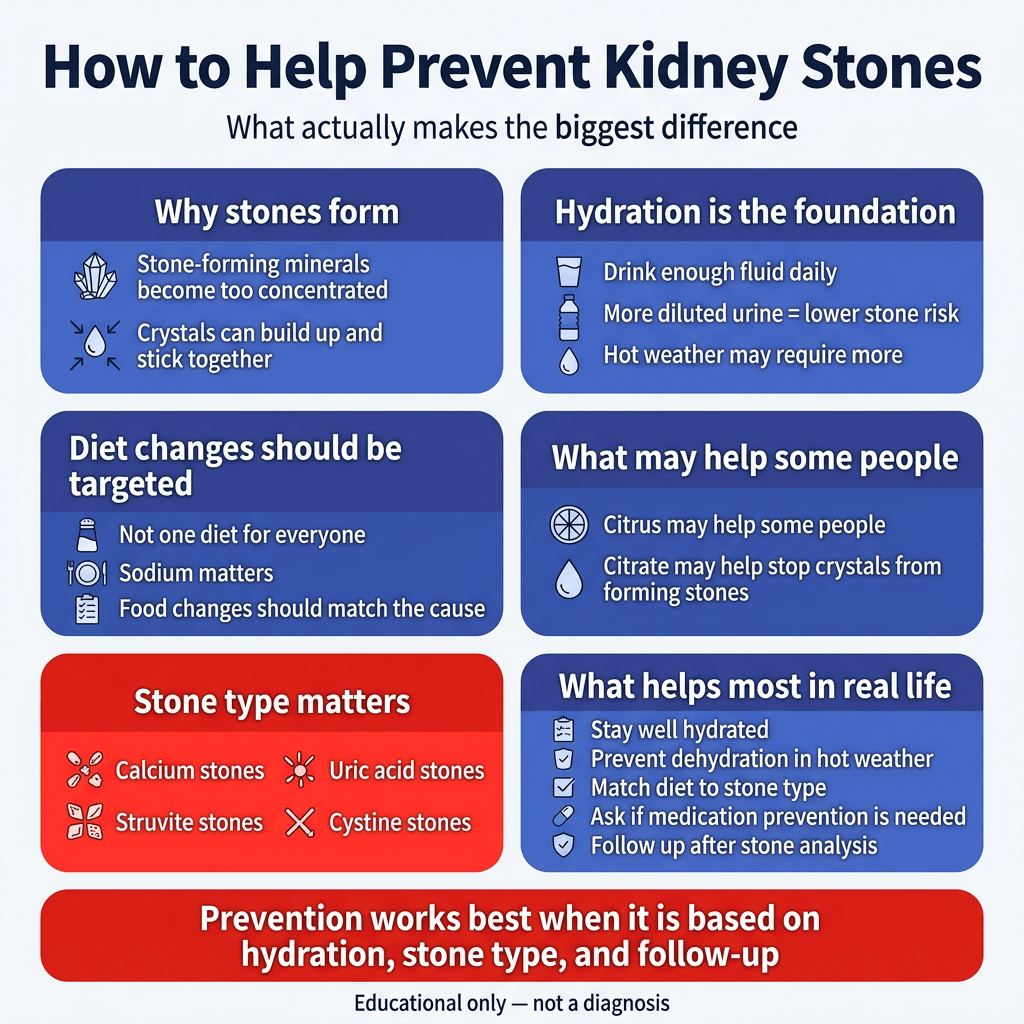
- drink enough fluid daily and more when sweating more heavily
- avoid letting dehydration become routine, especially in hot weather
- make food changes based on your stone type and clinician guidance, not random internet lists
- ask whether you need medication prevention if stones are recurring
- treat and follow up on infections properly if infection-related stones are part of the picture
Warning symptoms that shouldn’t wait
Prevention is usually an outpatient conversation. But if you think you may have a current stone problem and you also have any of the following, it should not be delayed:
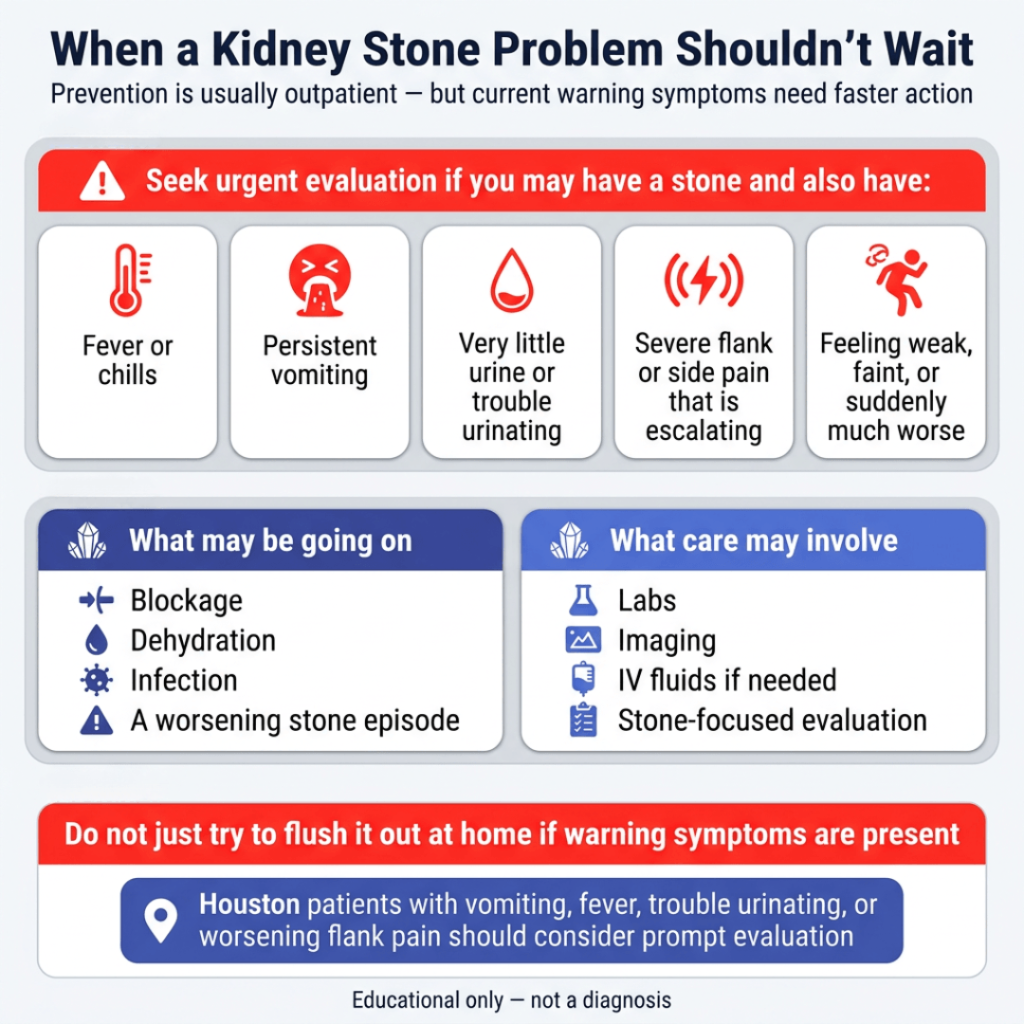
- fever or chills
- persistent vomiting
- very little urine or trouble urinating
- severe flank or side pain that is escalating
- feeling weak, faint, or suddenly much worse
NIDDK’s kidney-stone guidance says stones can become a more urgent problem when symptoms worsen or when there may be blockage, and its treatment page notes that vomiting and dehydration can require IV fluids. The broader kidney-stone symptom pages also identify fever/chills and trouble urinating as important warning signs.
If you’re in Houston and you think you may be dealing with a current kidney stone episode—especially if it involves vomiting, fever/chills, trouble urinating, or worsening flank pain—it’s reasonable to get checked promptly rather than wait for it to escalate.
Post Oak ER states it is a 24/7 emergency room in Houston’s Post Oak & Galleria area with board-certified ER physicians, plus on-site CT, ultrasound, X-ray, and labs. Its near-Houston page also notes convenient access near The Galleria and Uptown Park and that patients often come from areas such as Uptown, the Energy Corridor, Westchase, Midtown, and the Heights.
Frequently Asked Questions
Does drinking water really prevent kidney stones?
Yes — for most people, higher fluid intake is one of the most important prevention strategies. NIDDK states that drinking enough liquid every day is the best way to help prevent most kidney stones.
Is lemonade good for kidney stone prevention?
Sometimes. NIDDK notes that some studies suggest citrus drinks may help because citrate can stop crystals from becoming stones.
Can kidney stones come back?
Yes. Recurrent stones are common enough that prevention planning matters, especially after the first stone has been identified and analyzed. NIDDK’s prevention guidance is specifically built around reducing recurrence.
Are all kidney stone prevention diets the same?
No. Prevention works best when it is based on the stone type and the person’s risk factors, not one generic food list.
When should I go in instead of trying to “flush it out” at home?
If you have fever, vomiting, trouble urinating, or severe worsening pain, it should not be delayed.

