Key Takeaways
- Chronic hypertension is long-term high blood pressure that can damage arteries quietly, even when you feel normal.
- Over time, that vessel damage can make arteries more likely to clog or burst, which raises risk for both major stroke pathways.
- Stroke isn’t something you should “wait and see” on. If symptoms look like stroke, call 911 right away.
- In Harris County (Houston area), 28.0% of adults reported being told they have high blood pressure (BRFSS 2021; portal updated Jan 2024).
What chronic hypertension actually means
When patients tell me, “Doc, my blood pressure is high sometimes,” I usually ask one follow-up: high sometimes… or high most of the time and you only catch it sometimes?
Chronic hypertension is about a pattern, not a single reading:
- readings that are consistently above the healthy range over time
- or readings that are frequently high enough that your clinician considers it hypertension and starts treating it as a long-term condition
does chronic hypertension cause stroke?
Yes—chronic hypertension is one of the biggest drivers of stroke risk because it slowly changes the condition of your blood vessels. When pressure runs high for months and years, arteries can become more prone to clogging and more prone to rupturing.
Here’s the part that catches people off guard: you can feel totally fine while that damage is happening. The American Stroke Association literally calls high blood pressure “the silent killer” because many people don’t notice symptoms until something serious occurs.
So if you’ve had high blood pressure for a long time—even if it’s “only sometimes high”—this is worth taking seriously before your body forces the issue.
Chronic hypertension vs a one-off spike
A stressful day, too much caffeine, pain, lack of sleep—those can bump your numbers up temporarily. Chronic hypertension is different: it’s the pressure your vessels are living under week after week, month after month.
Chronic hypertension vs hypertensive emergency
Another common confusion: chronic risk vs right-now danger.
The American Stroke Association includes a “hypertensive emergency” concept—very high readings with symptoms like chest pain, shortness of breath, numbness/weakness, vision changes, or difficulty speaking—where the instruction is to call 911.
That matters because some people think, “My blood pressure is high, but I’ll just lie down and see.” If the symptoms suggest stroke or a hypertensive emergency picture, don’t negotiate—get help.
How long-term high blood pressure damages blood vessels
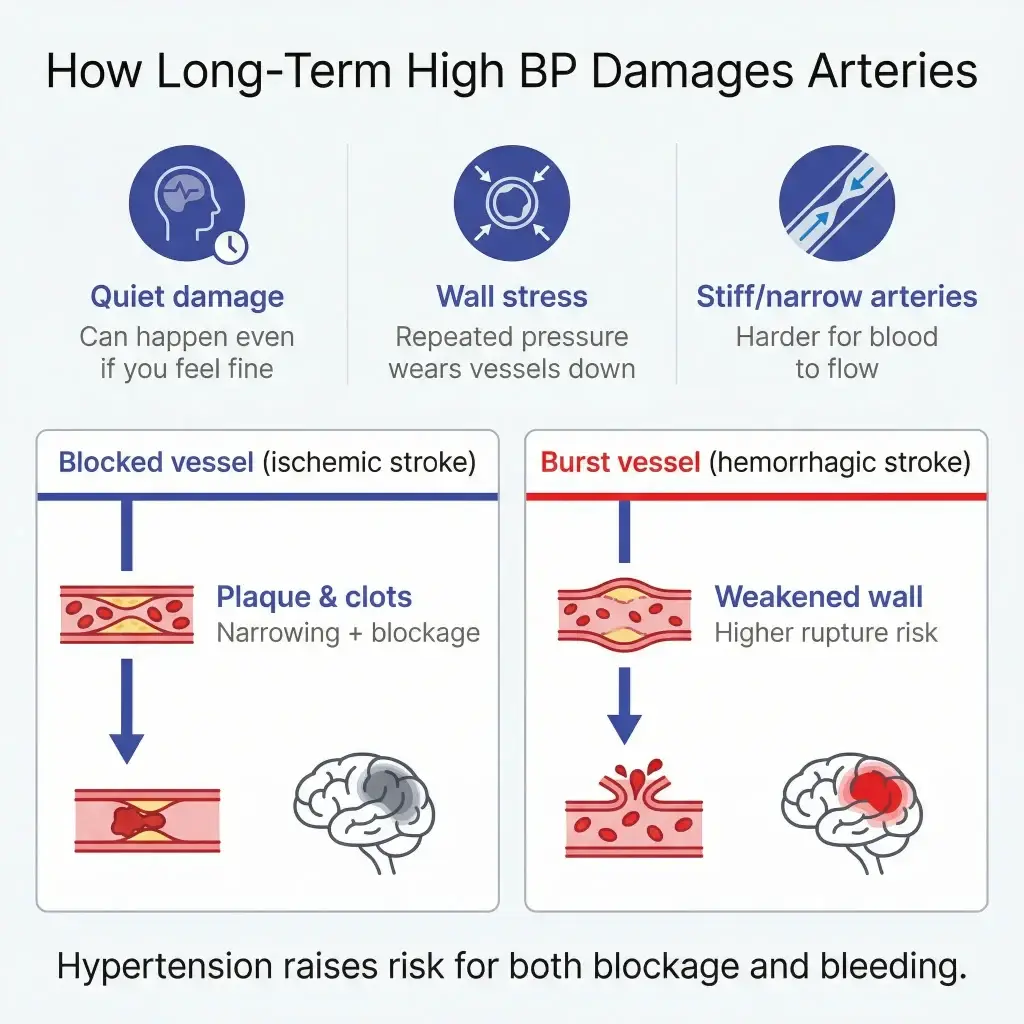
This is the “why” behind all the warnings.
Wear-and-tear on artery walls
Your arteries aren’t rigid pipes; they’re living tissue. When pressure is high over time, the vessel wall takes repeated stress. The American Heart Association explains that high blood pressure damages arteries and creates conditions that make arteries burst or clog more easily.
The American Stroke Association describes the mechanism in a simple way: excess pressure can stretch arteries beyond a healthy limit and cause small tears; the “repair” process can contribute to changes in the vessel wall that set the stage for plaque, clots, and hardened/weakened arteries.
Why plaque and clots become more likely
Hypertension doesn’t work alone. It often teams up with things like high cholesterol, diabetes, smoking, and inactivity. Over time, vascular injury and inflammation make the environment more favorable for atherosclerosis (plaque buildup) and for clot formation that can block blood flow.
Why hypertension also raises bleeding risk in the brain
Not every stroke is a blockage. Some strokes happen when a vessel ruptures and bleeds in or around the brain. High blood pressure increases stress on vessel walls, and weakened vessels are more vulnerable.
This is why “how hypertension causes stroke” isn’t just one story. It’s two.
The two big stroke pathways hypertension affects
Ischemic stroke (blocked blood flow)
An ischemic stroke happens when a brain blood vessel is narrowed or blocked—often by a clot.
Hypertension contributes by damaging vessels and making the conditions for blockage more likely over time.
Hemorrhagic stroke (bleeding in/around the brain)
A hemorrhagic stroke happens when a blood vessel ruptures in or near the brain.
Long-term high pressure can weaken vessels, raising vulnerability to rupture.
Stroke symptoms: what matters most in the moment

Let’s keep this practical: people waste time because they’re trying to decide whether they’re “sure.”
You don’t need to be sure. You need to recognize the pattern.
The CDC lists common stroke symptoms as sudden:
- numbness or weakness in the face/arm/leg (especially one side)
- confusion, trouble speaking, trouble understanding
- trouble seeing
- trouble walking, dizziness, loss of balance/coordination
- severe headache with no known cause
When to call 911
If you suspect stroke—especially sudden one-sided weakness, face droop, speech trouble, sudden vision loss, sudden balance trouble, or sudden severe headache—Call 911 for severe symptoms / suspected stroke.
“Is it my blood pressure or is it stroke?”
- A stroke usually declares itself with neurologic changes (face/arm/speech/vision/balance), often sudden.
- If your symptoms are neurologic, don’t get distracted by the blood pressure number. Treat the symptoms as the emergency.
Who is most at risk when hypertension is chronic?
Chronic hypertension doesn’t usually show up alone. It tends to stack with other risk factors—and the stacks are what drive risk up.
The American Stroke Association lists multiple factors that increase risk for high blood pressure, including age, family history, lack of physical activity, poor diet, obesity, and too much alcohol.
And from a prevention standpoint, NINDS emphasizes blood pressure control as a central strategy for preventing stroke.
The “I didn’t know I had it” problem
This is why routine checks matter. High blood pressure often has no obvious symptoms, which is exactly why it causes damage quietly.
And locally, this isn’t abstract: again, in Harris County (Houston area), 28.0% of adults reported being told they have high blood pressure (BRFSS 2021).
What to do right now
If symptoms are happening now
If you or someone with you has stroke symptoms (sudden face/arm weakness, speech trouble, vision changes, balance issues, sudden severe headache), Call 911 right away.
If your blood pressure is extremely high and you have symptoms like chest pain, shortness of breath, weakness/numbness, vision change, or difficulty speaking, that’s also an emergency situation—call 911.
If you’re stable but worried about long-term risk
If you’re not having emergency symptoms, this is where you can actually reclaim control:
- Start tracking readings consistently (same time of day, same conditions) and bring the trend to your clinician.
- Don’t build your entire plan around one “good” week or one “bad” day—look for patterns.
- Work with your clinician on a plan you can maintain (lifestyle + medication decisions when appropriate). The American Stroke Association emphasizes home monitoring and regular interaction with your care team.
- Lean into the basics that move the needle: lower sodium, more fruits/vegetables (potassium), and regular physical activity—NINDS highlights these in stroke prevention guidance.
What to expect in an ER evaluation for possible stroke
If someone comes in with possible stroke symptoms, ER teams focus on speed and clarity:
- When did symptoms start? (or when was the person last normal?)
- focused neurologic exam
- ruling out dangerous causes quickly
The exact workup depends on the symptoms, timing, and initial exam findings. The key point is that stroke evaluation is time-sensitive, so emergency care is designed to move quickly.
How to prevent a stroke when you’ve had high blood pressure for years
This is where chronic hypertension becomes a long game—and the good news is, prevention is not mysterious. It’s just consistent.
Blood pressure control basics (high-level)
The American Heart Association is blunt: you can reduce your risk for stroke by managing high blood pressure.
The American Stroke Association lists practical actions: healthy weight, DASH-style eating, reduce salt, physical activity, avoid tobacco, sleep, stress management, limit alcohol, and take medication as prescribed.
The lifestyle “big levers” that actually move risk
If you want a practical starting list you can live with:
- Salt awareness (most sodium is hidden in packaged food)
- Regular movement (consistency beats intensity)
- Sleep (poor sleep drives BP up for many people)
- Weight trend (even modest improvements help)
- Avoid tobacco
NINDS also highlights cutting down on salt, eating fruits and vegetables, exercising more, and controlling blood pressure as stroke prevention fundamentals.
Don’t Wait on Stroke Symptoms
If you notice sudden face drooping, arm weakness, speech trouble, vision changes, balance problems, or a severe headache, treat it like an emergency. Call 911 right away. Stroke care is time-sensitive, and waiting to “see if it passes” can cost critical treatment time.
If you’re worried about very high blood pressure, stroke symptoms, or other severe neurologic changes, Post Oak ER is open 24/7 for emergency evaluation. And if stroke is suspected, do not drive yourself—call 911 for immediate transport.
Need emergency care now? Visit Post Oak ER.
Think it could be a stroke? Call 911 immediately.
Frequently Asked Questions
Does hypertension cause stroke?
Yes—hypertension damages arteries and creates conditions that make arteries more likely to clog or burst, increasing stroke risk.
How does hypertension cause stroke over time?
Through long-term vessel damage: stiffening and injury to artery walls, higher likelihood of blockage, and higher vulnerability to rupture.
Can high blood pressure cause a stroke even if I feel fine?
Yes. High blood pressure often has no obvious symptoms, which is why it’s called the “silent killer.”
What are the signs of a stroke I should never ignore?
Sudden face/arm/leg weakness (especially one-sided), sudden speech trouble, sudden vision trouble, sudden balance trouble, or sudden severe headache. The CDC’s instruction is to call 911 immediately for these symptoms.
When should I call 911?
If stroke is suspected—or symptoms are severe and sudden—call 911 right away.
If I’ve had high blood pressure for years, can I still lower my stroke risk?
Yes. Major stroke-prevention guidance emphasizes that controlling blood pressure and improving lifestyle factors reduces risk.
Visit Post Oak ER (open 24/7).
Call 911 for severe symptoms.