Noticing a new spot on your skin can mess with your head fast. A mole that looks “different,” a sore that won’t heal, a tiny bump that keeps bleeding when you wash your face—your brain goes straight to the worst-case scenario.
Most skin changes are not cancer. But some are worth taking seriously, quickly—especially when the spot is new, changing, bleeding, or not healing.
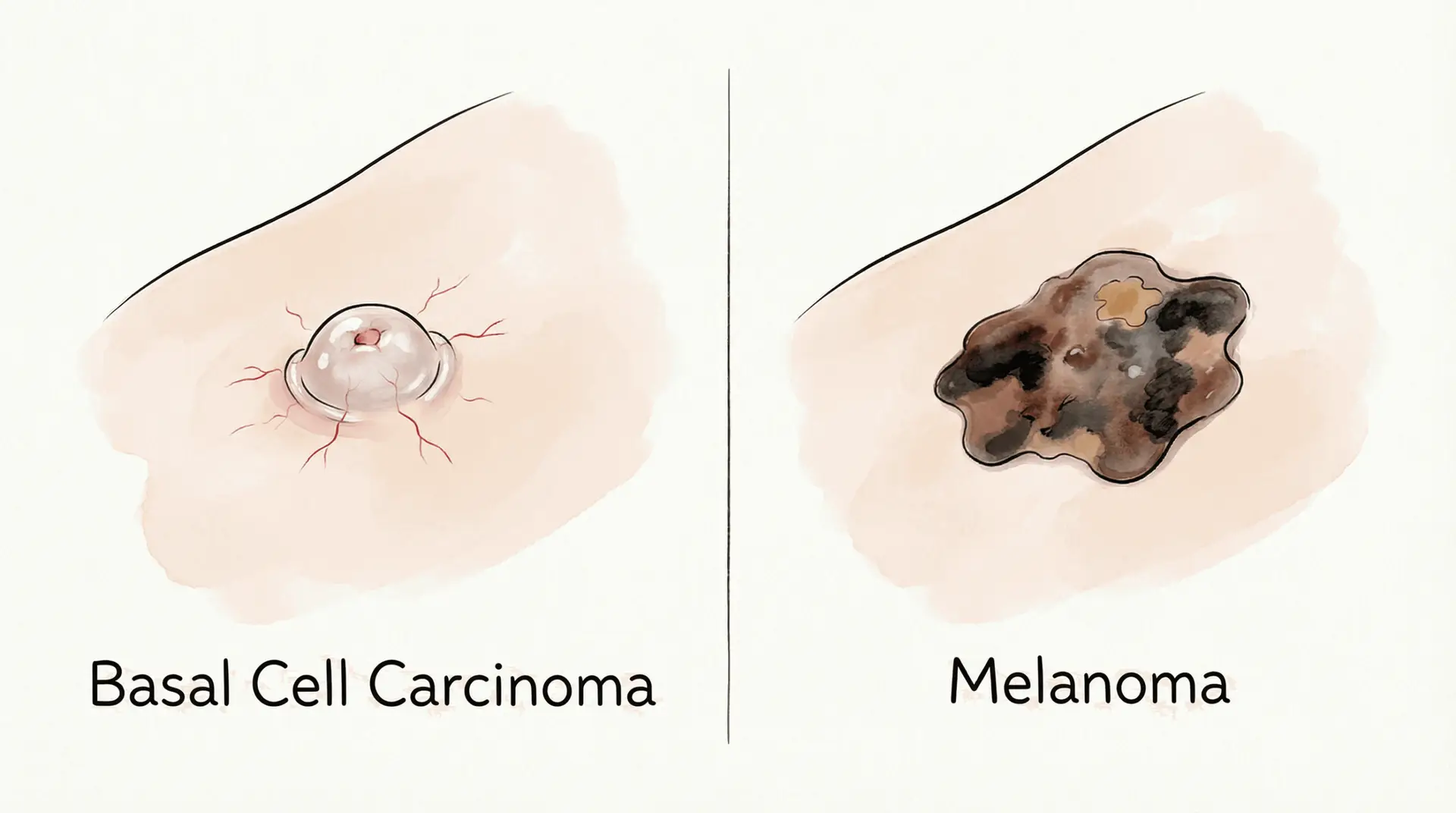
This guide breaks down basal cell carcinoma vs melanoma in plain language: what they are, what they can look like, who’s more at risk, and which symptoms are “don’t wait” red flags.
What this means
Basal cell carcinoma (BCC) and melanoma are both types of skin cancer, but they behave very differently.
- Basal cell carcinoma is the most common skin cancer. It usually grows slowly and is often handled by a dermatologist with a procedure to remove it. It rarely spreads to distant parts of the body, but it can grow into nearby tissue and cause serious local damage if ignored.
- Melanoma is less common, but it’s the one clinicians take extremely seriously because it’s more likely to spread (metastasize) if it isn’t found and treated early.
If you remember one thing, make it this:
Melanoma is usually the higher “spread risk.” BCC is usually the higher “local damage if ignored” risk.
Symptoms and appearance: what you might notice
Skin cancer doesn’t have one “look.” It can be subtle. It can mimic a rash, a scar, a pimple, or a harmless mole. The pattern that matters most is new + changing.
What basal cell carcinoma often looks like
Basal cell carcinoma often shows up in areas that get a lot of sun exposure (think face, ears, neck), and it can look like:
- A shiny or pearly bump
- A pink / skin-colored growth
- A flat, scaly patch
- A spot that looks like a scar (waxy, pale, or firm)
- A sore that keeps crusting, bleeding, then “almost healing,” then coming back
BCC may not hurt early. As it enlarges, symptoms like itching, bleeding, or pain can happen.
If you’ve been wondering “what is a basal cell carcinoma skin cancer”—think of it as a skin cancer that starts in the basal cells (lower part of the epidermis) and often grows slowly, especially on sun-exposed areas.
What melanoma often looks like
When people ask “what does melanoma skin cancer look like?” the most common answer is: it often looks like a new or changing mole—or a spot that just looks “off” compared to the rest.
The classic self-check is the ABCDEs:
- A — Asymmetry: one half doesn’t match the other
- B — Border: irregular, jagged, or blurry edges
- C — Color: multiple colors or uneven color
- D — Diameter: often larger than a pencil eraser (but not always)
- E — Evolving: changing in size, shape, color, or symptoms
The American Cancer Society also flags changes in how a spot looks or feels—including itching, tenderness, bleeding, or crusting—as reasons to get checked.
the “ugly duckling” idea—one mole looks different from all your other moles. If it stands out, it deserves attention.
A quick note about skin tone
Melanoma and other skin cancers can appear in all skin tones. In darker skin, melanoma may show up in less sun-exposed areas (like palms, soles, or under nails), and it may not look like the “classic” images people see online. If a spot is new, changing, bleeding, or not healing, trust that signal and get evaluated.
Which is more dangerous?
Here’s the cleanest way to frame it:
- Melanoma earns urgency because it has a higher chance of spreading if missed.
- Basal cell carcinoma is often very treatable, but if you ignore it long enough, it can grow deeper and damage nearby tissue (especially on the face). It very rarely spreads far, but it can still become serious if untreated.
Both should be taken seriously. One is more known for spread (melanoma). The other is more known for local destruction if delayed (BCC).
Who is more at risk (risk factors)
Risk is not about “deserving” cancer—it’s about exposure + biology + time.
Common risk factors discussed by major public health and cancer sources include:
- UV exposure (sun, tanning beds, sunlamps)
- History of sunburns, especially repeated burns
- Indoor tanning (tanning beds are a major UV source)
- Lots of moles or atypical moles
- Personal or family history of skin cancer
- Weakened immune system
- Older age (more cumulative UV exposure)
The big theme is UV exposure. The CDC and NCI both emphasize that UV radiation from the sun and tanning devices can damage skin cells and increase skin cancer risk.
You don’t need to memorize a checklist. If you’ve had heavy sun exposure over the years (work, hobbies, childhood sunburns), or you’ve used tanning beds, your “get suspicious spots checked” threshold should be lower.
Texas context: how common is melanoma here?
Melanoma is tracked through cancer registries, but basal cell carcinoma usually is not. That’s why you’ll often see clean incidence numbers for melanoma, and less precise statewide reporting for BCC.
From the State Cancer Profiles data (NCI/CDC), Texas’ melanoma incidence rate was 15.4 cases per 100,000 people (2018–2022, age-adjusted).
If you want county-level melanoma stats (Harris County included), the Texas Cancer Registry points people to tools like TxCanViz and the CDC’s U.S. Cancer Statistics Data Visualizations for local breakdowns.
Go to the ER now (red flags you shouldn’t wait on)
Most suspicious skin spots are best evaluated urgently by a primary care clinician or dermatologist—but there are situations where an ER visit is appropriate.
Seek emergency care now if you have a concerning skin lesion plus any of the following:
- Uncontrolled bleeding from a mole/spot/wound that won’t stop with firm pressure
- Rapidly spreading redness, warmth, swelling, or pus (possible infection), especially with fever
- Severe or rapidly worsening pain at the site
- A lesion with surrounding skin that looks blackened, severely blistered, or suddenly deteriorating
- You feel systemically ill (fever, weakness, confusion) along with a worsening skin lesion
Worried about a skin spot that’s bleeding, painful, infected, or suddenly changing? Don’t wait on emergency warning signs. Visit Post Oak ER — Open 24/7 for prompt evaluation and care.
What doctors may do next
A clinician can’t confirm melanoma or basal cell carcinoma just by guessing—confirmation usually requires a biopsy.
Here’s what the evaluation commonly looks like:
- Visual exam and history (how long it’s been there, changes over time, symptoms)
- A closer look (often by dermatology) with tools to examine skin features more clearly
- Skin biopsy (removing a small sample to test it in a lab)
The American Cancer Society describes biopsy as a key step when a spot might be melanoma, and similarly notes that a biopsy may be done to confirm basal/squamous cancers.
Any next steps (removal type, follow-up, staging) depend on the biopsy findings—so the goal is to get the right spot assessed and tested, not to self-diagnose at home.
What you can do today
You don’t need panic. You need a plan.
Do a calm self-check
- Look for new, changing, or unusual spots.
- Use the ABCDE method for moles.
- Pay attention to “won’t heal” areas too—especially on sun-exposed skin.
Take a clear photo
- Good lighting, same angle, include a ruler/coin for size reference.
- Date it. This helps you and your clinician track “E = evolving.”
Reduce UV exposure going forward
- Make sun protection routine and avoid tanning beds/sunlamps.
- UV rays can still hit you on cloudy days; habits matter more than “once in a while.”
Frequently Asked Questions
How can you tell the difference between basal cell carcinoma and melanoma?
You can’t confirm the difference just by looking—but you can spot patterns:
BCC often looks like a pearly/shiny bump, a scaly patch, or a sore that doesn’t heal.
Melanoma often looks like a new or changing mole and may show ABCDE changes.
Either way, confirmation typically requires a clinician evaluation and often a biopsy.
Can basal cell skin cancer turn into melanoma?
Generally, they are different cancers from different cell types. BCC doesn’t “turn into” melanoma—but a person can develop more than one type of skin cancer over time.
If you have a new suspicious spot, treat it as its own issue and get it evaluated.
Does basal cell skin cancer spread?
Basal cell skin cancers very rarely spread to distant parts of the body, but they can grow into nearby tissues and cause serious problems if not treated.
What does melanoma skin cancer look like?
Often: a new mole or a mole that is changing (ABCDE: asymmetry, border irregularity, color variation, diameter, evolving).
How fast does melanoma skin cancer spread?
There isn’t one timeline. The risk of spread depends on factors like how deep the melanoma is and whether it has been growing unnoticed. What matters practically: don’t wait on a changing/bleeding spot—prompt evaluation is how melanoma is caught early.
Is basal cell skin cancer dangerous?
It can be—especially if ignored. It’s usually very treatable, and it rarely spreads far, but it can still cause significant local damage if it grows into nearby tissue.