Key Takeaways
- A stroke is an emergency in the brain—either a blocked artery or a ruptured/bleeding artery.
- A heart attack is an emergency in the heart muscle, usually from a blocked coronary artery.
- They can feel similar in the moment (sweating, nausea, “something’s wrong”), but the classic warning signs are different.
- If you suspect stroke, call 911 right away.
is a stroke the same as a heart attack?
No—they’re not the same, but they’re related in one important way: both are blood-flow emergencies and both need fast action.
- A stroke happens when blood flow to part of the brain is blocked or there is bleeding in the brain.
- A heart attack happens when blood flow to part of the heart muscle is blocked, damaging the heart muscle.
The simplest difference: brain vs heart
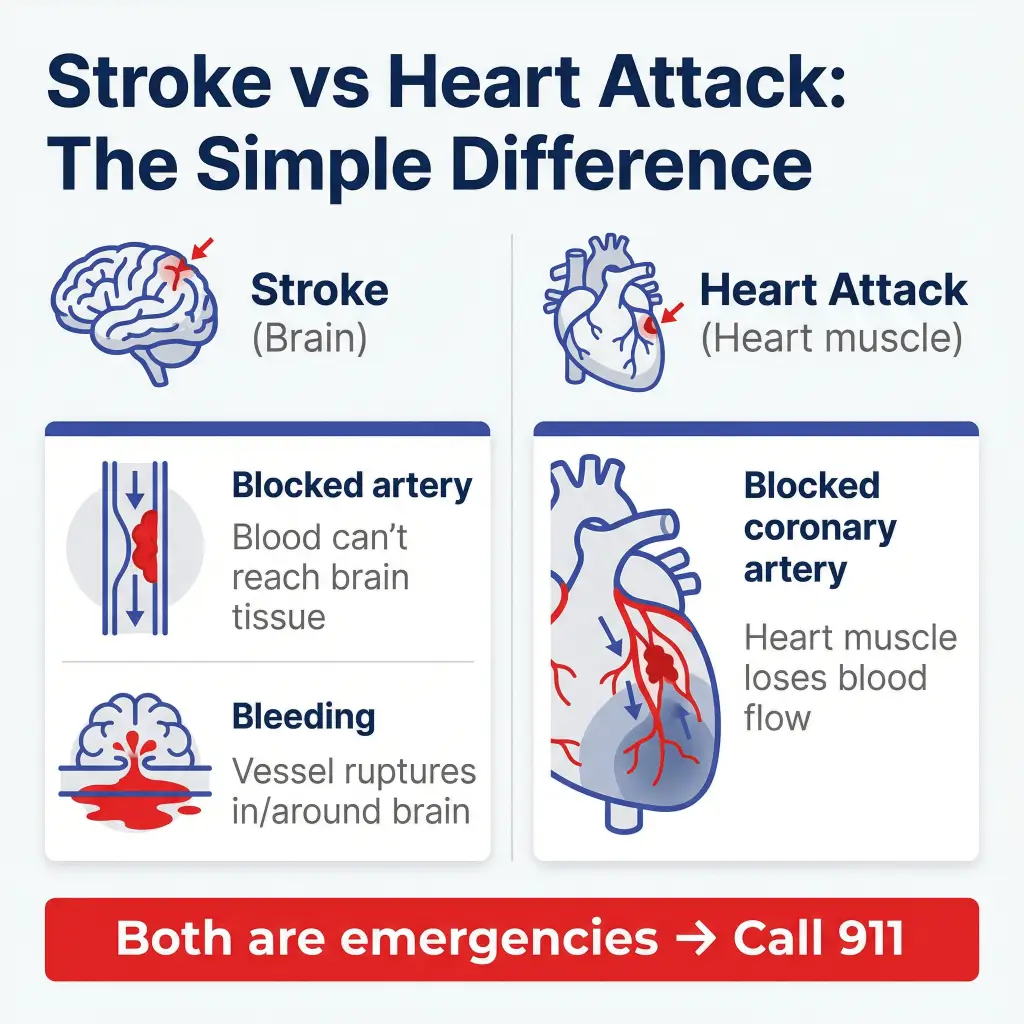
Stroke (brain)
The CDC describes stroke as a “brain attack” that happens from a blocked artery or a ruptured artery.
NHLBI explains the consequence plainly: when the brain can’t get oxygen and nutrients, brain cells begin to die within minutes.
Heart attack (heart muscle)
NHLBI lists heart attack symptoms and makes clear that it’s a heart emergency—often involving chest discomfort and other signs, and it can happen even with mild or no symptoms in some people.
Why people confuse stroke and heart attack
Three reasons I see all the time:
- Both can come on suddenly and feel scary.
- Both can share “general” symptoms like sweating, nausea, dizziness, anxiety.
- People focus on the wrong detail (“Is it pain?”) instead of the pattern (“Is this neurologic? Is this chest pressure + shortness of breath?”).
Warning signs: stroke symptoms vs heart attack symptoms

Stroke warning signs
The CDC’s stroke warning signs are about sudden neurologic change, including: sudden one-sided weakness/numbness, trouble speaking/understanding, trouble seeing, trouble walking/balance, and sudden severe headache with no known cause.
Heart attack warning signs
The American Heart Association lists warning signs including chest discomfort, discomfort in other upper body areas (arm/back/neck/jaw), and shortness of breath, among others.
NHLBI also lists symptoms such as chest pain/heaviness, arm/back/neck/jaw discomfort, shortness of breath, sweating, unusual fatigue (noted as more common in women), nausea/vomiting, dizziness, and rapid/irregular heartbeat.
If you have chest pain/pressure or heart attack warning signs, treat it as an emergency and call 911.
Overlap symptoms that confuse people
Some symptoms can happen in either emergency:
- sweating, nausea/vomiting, dizziness/lightheadedness, anxiety, sudden fatigue
That overlap is exactly why trying to self-diagnose can be dangerous. The better rule is: recognize red flags and act.
What should you do if you’re not sure which one it is?
Here’s the simplest guidance:
- If you suspect stroke (sudden face/arm weakness, speech trouble, sudden vision/balance changes): call 911 immediately.
- If you suspect heart attack (chest pressure/discomfort ± shortness of breath, sweating, nausea, radiating discomfort): call 911 immediately.
The CDC is explicit for stroke: call 9-1-1 right away.
And the American Stroke Association reinforces: call 911 even if you observe just one stroke symptom.
Can a heart attack cause a stroke?
It can—in a few well-known ways.
Clot formation after a heart attack
After certain heart attacks, a clot can form inside the heart and travel to the brain. Cleveland Clinic describes “left ventricular thrombus” as a clot in the lower left chamber that can break free and travel through arteries, leading to a stroke.
Shared root causes (the “same plumbing problem”)
Atherosclerosis (plaque buildup) is a common root problem that contributes to both heart attacks and strokes. The American Stroke Association describes atherosclerosis as plaque buildup in arteries that can lead to heart disease and stroke.
Heart conditions that throw clots
CDC notes that coronary artery disease increases stroke risk (plaque buildup can block oxygen-rich blood flow), and other heart conditions—like irregular heartbeat (including AFib) and enlarged heart chambers—can form clots that break loose and cause stroke.
So the short answer: they’re different emergencies, but the heart and brain are connected through the same circulation system—and problems in one can raise risk in the other.
“Which is worse—stroke or heart attack?”
I understand why people ask. But medically, it’s not a clean ranking.
- Some strokes are small; some are devastating.
- Some heart attacks are mild; some cause sudden cardiac arrest.
What matters is this: both can be deadly or permanently disabling, and both have outcomes that improve when you act fast.
If you’re choosing between “maybe I’m embarrassed” and “maybe I’m late,” choose embarrassment. Every time.
What to expect in the ER
If clinicians suspect stroke
- They’ll focus on timing (when symptoms started / last-known-well), because stroke care is time-sensitive.
- They’ll do a focused neurologic exam and evaluate for blocked blood flow vs bleeding. (Stroke can be a blocked artery or ruptured/bleeding artery.)
If clinicians suspect heart attack
- Expect rapid assessment of symptoms and heart rhythm plus testing based on clinical judgment. NHLBI’s symptom guidance reflects how broad presentations can be—including atypical symptoms like unusual fatigue, nausea, or dizziness.
Prevention basics
If you want to reduce risk for both stroke and heart attack, you’re usually targeting the shared drivers:
- blood pressure control
- diabetes control
- smoking cessation
- cholesterol/atherosclerosis risk management
And one more practical prevention tip: learn the warning signs. NIH’s News in Health makes the point clearly—recognizing symptoms and getting treatment fast can mean the difference between life and death or disability.
When Every Minute Matters, Get Emergency Help Fast
If you notice sudden stroke symptoms like one-sided weakness, trouble speaking, vision changes, loss of balance, or a severe headache, call 911 immediately. If you have heart attack warning signs like chest pressure, shortness of breath, sweating, nausea, or pain spreading to the arm, back, neck, or jaw, call 911 right away.
At Post Oak ER, we’re open 24/7 to evaluate emergency symptoms and help you get rapid medical attention when something feels seriously wrong. If symptoms are severe or you think it could be a stroke or heart attack, do not wait and do not drive yourself if you’re unsafe to do so—call 911.
Frequently Asked Questions
Is a stroke the same as a heart attack?
No. Stroke affects the brain (blocked blood flow or bleeding). Heart attack affects the heart muscle (often from a blocked coronary artery).
What’s the difference between a stroke and a heart attack?
Stroke = brain blood flow blocked or bleeding. Heart attack = heart muscle blood flow blocked and muscle is injured.
Is a stroke a heart attack?
No—different organs and different mechanisms. But both are vascular emergencies that require urgent care.
Can a heart attack cause a stroke?
It can. A clot can form in the heart after some heart attacks and travel to the brain, causing stroke.
What are the signs of a stroke I should never ignore?
Sudden one-sided weakness/numbness, speech trouble, vision trouble, balance trouble, or sudden severe headache—call 911 right away.
What are common heart attack warning signs?
Chest discomfort/pressure, discomfort radiating to arm/back/neck/jaw, shortness of breath, sweating, nausea, dizziness—call 911.
If I’m not sure which one it is, what should I do first?
Treat it as an emergency and call 911—especially for stroke-like neurologic symptoms or chest discomfort/shortness of breath.
Which is worse: heart attack or stroke?
Both can be fatal or disabling; the “worse” one is the one you delay treating. Act fast.
Can symptoms that go away still be serious?
Yes. A TIA (“mini-stroke”) can have temporary symptoms and still signals urgent risk; stroke can’t be ruled out early just because symptoms improve.