Key Takeaways
- A brain (cerebral) aneurysm is a weak spot in a brain artery that can bulge outward like a small balloon.
- Many unruptured aneurysms cause no symptoms, but some can press on nearby nerves and create warning signs.
- A ruptured aneurysm can cause bleeding around the brain (often subarachnoid hemorrhage) and is a sudden life-threatening emergency.
- If you suspect rupture—or you see sudden severe headache or sudden neurologic symptoms—Call 911 for severe symptoms.
What a brain aneurysm is
A cerebral (brain) aneurysm is a weak area in an artery wall that balloons outward and fills with blood. It can press on brain tissue or nerves, and it can rupture—releasing blood into or around the brain.
One reason this topic matters: brain aneurysms aren’t “one-in-a-million.” MedlinePlus (NIH) notes that about 1 in 50 people has a brain aneurysm, though only a small number rupture.
what are the signs of a brain aneurysm?
People searching for brain aneurysm signs are often asking about either:
- an unruptured aneurysm, which may be silent or cause subtle symptoms, or
- a ruptured aneurysm, which bleeds and becomes an emergency
That’s why aneurysm symptoms can be confusing. In some cases, they’re mild or vague. In others, they appear suddenly and dramatically.
The practical rule is simple: if symptoms are severe, sudden, or involve neurologic changes, treat it as an emergency rather than trying to figure it out at home. For severe symptoms, call 911.
Why it’s confusing: aneurysm vs stroke vs brain bleed
People often ask:
- Is an aneurysm a stroke?
- Is a brain aneurysm a stroke?
- Is a brain bleed a stroke?
- What’s the difference between a stroke and an aneurysm?
Here’s a clean way to think about it:
- An aneurysm is a problem in the vessel wall (a weak, bulging spot in an artery).
- A stroke is brain injury from interrupted blood flow or bleeding. Stroke can be ischemic (blocked vessel) or hemorrhagic (bleeding).
- A brain bleed is bleeding inside/around the brain. Some brain bleeds fall under the hemorrhagic stroke umbrella.
A ruptured brain aneurysm can cause bleeding around the brain (often aneurysmal subarachnoid hemorrhage), which is treated as a stroke-type emergency—but the aneurysm itself is not “the same thing” as stroke.
Unruptured vs ruptured aneurysm
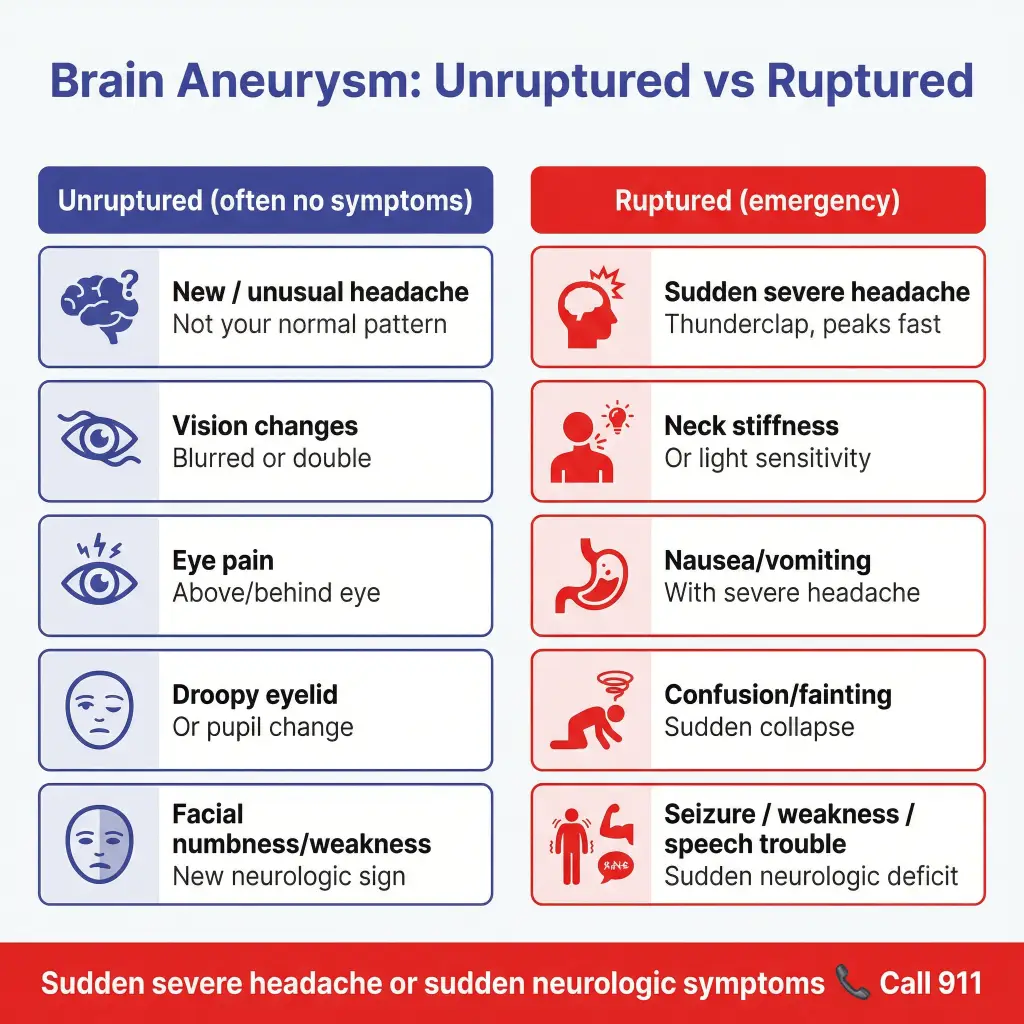
- Unruptured aneurysm: Often silent. Sometimes causes symptoms if it presses on nearby nerves or structures.
- Ruptured aneurysm: Causes bleeding and can become life-threatening quickly. The American Heart Association describes aneurysmal subarachnoid hemorrhage as a sudden, life-threatening emergency.
Signs of an unruptured brain aneurysm
many unruptured aneurysms cause no symptoms and are discovered incidentally on imaging done for another reason.
But when an unruptured aneurysm does cause symptoms, it’s usually because it’s irritating or compressing nearby nerves.
Headache patterns that deserve attention
Most headaches are not aneurysms. But these patterns deserve medical attention because they’re outside a person’s normal baseline:
- A headache that is new, unusual, or worsening compared to your typical headaches
- Headache plus new neurologic symptoms (vision changes, droopy eyelid, facial numbness)
- Headache that’s persistent and doesn’t behave like your usual pattern
Eye and vision-related symptoms
Some unruptured aneurysm symptoms can involve the eye/face area because of where certain aneurysms sit and which nerves they might affect. Symptoms can include:
- Vision changes (blurred or double vision)
- Pain above or behind the eye
- A drooping eyelid
- A change in pupil size
These are not “aneurysm-proof” symptoms—but they are meaningful red flags, especially if they show up suddenly or are clearly new.
Neurologic symptoms you shouldn’t brush off
If you notice sudden neurologic changes, don’t talk yourself out of it. Examples include:
- New weakness or numbness (especially one-sided)
- New difficulty speaking or understanding speech
- Sudden trouble walking or balancing
- Sudden confusion
Those overlap with classic stroke symptoms, and stroke itself is defined as blocked blood flow to the brain or bleeding in the brain—both of which are emergencies.
Signs of a ruptured brain aneurysm
The sudden severe headache warning
A classic presentation is a headache that is:
- Sudden
- Severe
- Peaks very quickly (people often describe it as “out of nowhere”)
Clinicians often call this pattern a “thunderclap headache.” It doesn’t mean every severe headache is rupture—but this pattern is urgent enough that it should be treated seriously.
Other rupture red flags
A ruptured aneurysm can come with:
- Nausea or vomiting
- Neck pain or stiffness
- Light sensitivity
- Confusion, fainting, or decreased alertness
- Seizure
- Sudden neurologic deficits (speech problems, weakness, vision changes)
Different sources describe different clusters of symptoms, but the consistent message is the same: this is an emergency and needs rapid evaluation.
When to call 911
If you see any of the following, Call 911 for severe symptoms:
- A sudden, severe headache that is unlike anything you’ve felt before
- Sudden confusion, collapse, seizure, or loss of consciousness
- Sudden one-sided weakness, facial droop, slurred speech, or sudden vision loss
- A sudden “something is very wrong” neurologic change
You don’t need to prove it’s an aneurysm or a stroke. Your job is to recognize urgency and get emergency help. Stroke is a medical emergency because blocked blood flow or bleeding can damage brain tissue quickly.
Is an aneurysm a stroke? Can an aneurysm cause a stroke?
These questions show up constantly in real life, because people are trying to understand what category they’re in.
Is an aneurysm and stroke the same thing?
No. An aneurysm is a structural weakness/bulge in a blood vessel wall. Stroke is brain injury from blocked blood flow or bleeding.
Can an aneurysm cause a stroke?
A ruptured intracranial aneurysm can cause bleeding around the brain (subarachnoid hemorrhage), which is considered a type of hemorrhagic stroke event. JAMA Neurology notes that nontraumatic subarachnoid hemorrhage represents about 5% to 10% of all strokes, and that around 85% of nontraumatic SAHs are caused by rupture of an intracranial aneurysm.
So yes—aneurysm rupture can cause a stroke-type emergency. But “aneurysm” and “stroke” still aren’t interchangeable words.
Is a brain bleed a stroke?
Some brain bleeds fall under hemorrhagic stroke, which happens when a blood vessel ruptures and bleeds in or around the brain.
That said, clinicians also classify bleeds by where the blood is (in the brain tissue vs around the brain), why it happened, and what needs to happen next. The safest takeaway for a reader is simple: bleeding in or around the brain is urgent.
Who is more prone to brain aneurysm problems?
major references consistently discuss higher risk in people with factors like:
- High blood pressure
- Smoking
- Family history
- Certain inherited/connective tissue conditions (in some cases)
NINDS and Mayo Clinic discuss aneurysm formation and rupture risk in these terms (high-level), and they emphasize that aneurysms can rupture and cause serious outcomes.
What matters most from a practical standpoint
Here’s the real ER lens:
- If symptoms suggest rupture or stroke, we don’t “debate” risk factors—we act.
- Risk factors matter more in the prevention and follow-up phase than in the “do I need emergency care right now?” phase.
What to do right now
If symptoms are happening now
If someone is experiencing:
- sudden severe headache unlike prior headaches
- sudden neurologic deficits (face/arm/speech/vision/balance)
- collapse, seizure, or sudden confusion
Call 911 for severe symptoms.
Stroke is an emergency when blood flow is blocked or a vessel bursts, because brain tissue can become damaged quickly.
If you’re worried but stable
If you’re not having emergency symptoms but you’re worried because you’ve had:
- recurring unusual headaches
- new vision changes
- episodes of facial numbness or drooping
- intermittent neurologic symptoms
…don’t ignore it. Talk with a clinician promptly, and if symptoms escalate suddenly, treat it as an emergency.
This isn’t about panic. It’s about respecting patterns that are new and neurologic.
What to expect in the ER
If someone comes to the ER concerned about a possible stroke/bleed/aneurysm issue, the evaluation is usually focused and time-driven.
What clinicians focus on first
- When symptoms started (or when the person was last known well)
- A focused neurologic exam
- Vital signs and “immediate threats”
Typical evaluation tools
Depending on the presentation, clinicians often consider:
- Brain imaging (to look for bleeding or other urgent causes)
- Blood tests
- Heart rhythm evaluation (because some neurologic events can relate to rhythm issues)
The exact evaluation depends on the person’s symptoms, timing, and initial exam findings.
Don’t Wait on Sudden Neurologic Symptoms
When symptoms could be related to a brain aneurysm, stroke, or brain bleed, timing matters. A sudden severe headache, one-sided weakness, speech trouble, confusion, seizure, or sudden vision changes should be treated as an emergency.
Call 911 right away for severe symptoms.
For urgent symptoms that need prompt evaluation, Post Oak ER is open 24/7 and ready to assess emergency conditions such as severe headaches, neurologic changes, and possible stroke-related symptoms.
Visit Post Oak ER — Open 24/7
Call 911 for severe symptoms
Frequently Asked Questions
What are the most common signs of a brain aneurysm?
Many unruptured aneurysms cause u003cstrongu003eno symptomsu003c/strongu003e. When symptoms occur, they can include new headaches, vision changes, eye pain, or neurologic changes—especially if the aneurysm presses on nearby nerves.
Can you have a brain aneurysm with no symptoms?
Yes. This is common enough that aneurysms are often found incidentally on imaging done for other reasons.
What does a ruptured brain aneurysm feel like?
Classically: a u003cstrongu003esudden, severe headacheu003c/strongu003e that feels dramatically different from a typical headache, often with other red flags (nausea/vomiting, neck stiffness, confusion, fainting, seizure). It’s treated as a life-threatening emergency.
Is an aneurysm a stroke?
Not exactly. An aneurysm is a vessel-wall bulge; a stroke is brain injury from blocked blood flow or bleeding.
Is a brain aneurysm a stroke—or something different?
It’s different. But if a brain aneurysm ruptures, it can cause bleeding around the brain (aneurysmal subarachnoid hemorrhage), which is a stroke-type emergency.
Can an aneurysm cause a stroke?
Yes—rupture can lead to subarachnoid hemorrhage. Research summaries note that nontraumatic subarachnoid hemorrhage accounts for about u003cstrongu003e5%–10% of strokesu003c/strongu003e, and most are due to ruptured intracranial aneurysm.
What’s the difference between a stroke and an aneurysm?
Stroke = blocked blood flow or bleeding causing brain injury. Aneurysm = a weak, bulging spot in an artery wall that may never rupture—or may rupture and bleed.
Is a brain bleed a stroke?
Some brain bleeds fall under hemorrhagic stroke, which is bleeding in or around the brain from a ruptured vessel.
When is a headache serious enough to call 911?
If it’s u003cstrongu003esudden, severe, and unlike your usual headachesu003c/strongu003e, or it comes with neurologic symptoms, confusion, collapse, seizure, or vision/speech/weakness changes—u003cstrongu003eCall 911 for severe symptoms.u003c/strongu003e
Can aneurysm symptoms come and go?
Some warning symptoms (like intermittent headaches or vision issues) can fluctuate, but rupture symptoms are typically abrupt and severe. If neurologic symptoms come and go, that still warrants urgent medical evaluation because stroke/TIA patterns can also fluctuate.
Who is most at risk for a brain aneurysm?
Risk is higher in certain groups (e.g., high blood pressure, smoking, family history). But symptoms matter more than “fitting the profile.”
Can high blood pressure or smoking raise aneurysm risk?
They are commonly cited risk factors in major medical references discussing aneurysm formation/rupture risk.
What should I do if I’m worried I have an aneurysm but I’m stable?
Don’t self-diagnose or dismiss it. If symptoms are persistent or new (especially vision/neurologic changes), seek medical evaluation. If severe or sudden symptoms appear, treat it as an emergency.
What should I expect if I go to the ER for suspected aneurysm symptoms?
Expect focused questions about timing and symptoms, a neurologic exam, and evaluation aimed at ruling out dangerous causes (including bleeding). The exact plan depends on the situation and clinical findings.

